Luckily we are better informed today. As babies can’t tell us how much pain they are in, scientists have invented several ingenious methods to try and work out what they are feeling. But there’s still a remarkable amount we don’t understand. And our new study, published in Current Biology, shows that we may be underestimating how much pain babies feel when they are under stress.
The reason progress has been relatively slow is that there was for a long time no agreed method for reliably measuring babies’ pain perception. It’s only in the last few decades scientists have made increasing efforts to do this – and the results may be applicable to other people who are unable to communicate too.
The first clues came from animal models in the early 1980s. These showed that the structural and functional connections within the nervous system required to perceive a painful event are present from birth. However, we still do not know whether these connections are sufficiently mature for infants to experience pain in quite the same way as adults.
At the same time, clinical investigators started exploring ways of measuring pain in human infants. Following a painful procedure, such as the heel stick used for blood tests (much like a finger prick used for adult blood tests), infants show several significant responses. These range from physiological (changes in heart rate or breathing) and hormonal (release of the “stress hormone” cortisol) to behavioural (crying or grimacing).
Extensive research in this area suggested that infant pain should be evaluated with a combination of these measures, leading to the development of neonatal clinical pain scoring systems, such as the Premature Infant Pain Profile.
Pain in the brain
Another big advance in the field came from the Fitzgerald lab here at University College London, which moved away from solely using observations of behaviour and physiological responses to measure pain. Instead, it turned to the brain. We know that the perception of pain is generated by the central nervous system, so these researchers aimed to directly measure the activity of neurons (brain cells) that are responsible for the sensation of pain.
To do this, they used non-invasive measures like electromyography (EMG) and electroencephalography (EEG), which measure the electrical activity generated by muscles and brain cells, following a painful event. This method has the advantage of being both objective and quantitative, as it does not depend on observational scoring.
 These studies confirmed that infants do process pain in the brain, but that they differ in their experiences with age. First, the lab recorded spinal reflexes – such as the withdrawal reflex, which is intended to protect the body from damaging stimuli – and found that premature infants are more sensitive to sensory stimulation than older infants. They subjected babies to repeated non-painful touches, and found that younger infants moved their limbs following lighter touches than older infants. In fact, the older infants got used to the repeated touches and eventually stopped moving their limbs.
These studies confirmed that infants do process pain in the brain, but that they differ in their experiences with age. First, the lab recorded spinal reflexes – such as the withdrawal reflex, which is intended to protect the body from damaging stimuli – and found that premature infants are more sensitive to sensory stimulation than older infants. They subjected babies to repeated non-painful touches, and found that younger infants moved their limbs following lighter touches than older infants. In fact, the older infants got used to the repeated touches and eventually stopped moving their limbs.
They also found that premature infants responded to both painful and non-painful touch with whole body movements. In older babies (at term age, around 40 weeks) this matured into more a purposeful withdrawal of the stimulated limb, becoming more specific to pain rather than any touch.
An important next step was to record activity in the brain, which is where pain perception occurs. They did this with EEG, which uses electrodes placed on the scalp to track and record brain waves. They found that premature infants exhibited large bursts of brain activity which, as with early reflexes, are not specific to pain (a simple tap could produce a similar effect as a heel prick). Towards normal term age (a few weeks prior), infants were more likely to show a clear pain-specific brainwavesimilar to that seen in adults.
However, while this was a direct read out of what was happening in the nervous system after a painful event, you shouldn’t assume it was a direct reflection of what the baby was feeling. This is because the feeling of pain requires an emotional component as well as a sensory part, and although we can measure the sensory aspect, we can not measure or make assumptions about the emotional processing in a newborn.
Stress and pain
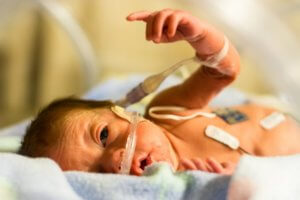
In our latest research, my colleagues and I at the Fitzgerald lab focused on stress and pain. Many infants experience physiological stress as a result of necessary clinical procedures. For example, hospitalised babies often require several painful procedures a day as part of their care, and those who do not will likely experience events such as being weighed or loud noises (alarms) as stressful.
For the first time, we measured both pain and stress at the same time as a single, clinically required blood test. In 56 hospitalised newborns, the pain-related brain activity and behavioural response was measured following the blood test, while the babies’ background level of stress was measured using the concentration of a stress hormone (cortisol) in the saliva and heart rate patterns.
The results show that for babies who are not stressed, a painful procedure will often result in a coordinated increase in brain activity and behaviour, in the form of facial expressions. Babies who are more stressed have an even larger response in the brain following a painful procedure, but, importantly, this is no longer matched by changes in behaviour. In other words, a stressed baby may have strong pain-related activity in their brain, but you could not tell that from simply observing their behaviour.
Since increased levels of stress can increase the amount of pain-related brain activity, it is clear that we should monitor and control the stress levels of hospitalised babies. Stressed babies may not seem to respond to pain although their brain is still processing it. The phenomenon has been seen in premature babies who sometimes “tune out” and become unresponsive when they are overwhelmed. But that doesn’t mean they are not experiencing something. Importantly, this means that doctors and nurses may underestimate their pain.
Given its huge importance, it may seem surprising that we know so little about what newborns actually feel. Thankfully, research is unravelling the mystery with impressive speed.
Laura Jones is a research associate in Neuro, Physiology and Pharmacology at University College London. She has a particular interest in the factors that can impact upon either the acute pain response or long term changes in their pain perception.
A version of this article was originally published on the Conversation as “The mystery of how babies experience pain” and has been republished here with permission.































