“The Phenotypic Characterization of the Cammalleri Sisters, an Example of Exceptional Longevity,” from Calogero Caruso M.D. of the University of Palermo, Italy, and colleagues, is published in Rejuvenation Research.
Filippa was a “semi-supercentenarian” of 106 years, born December 12, 1911 and who died July 6, 2018. Her sister Diega, born October 23, 1905 and who died June 15, 2019, was a supercentenarian, living until age 113. Among centenarians – those who see their 100th birthdays – only 1 in 1,000 makes it to 110. Only 27 supercentenarians are known in the world.
An article in The New Yorker, “Was Jeanne Calment the Oldest Person Who Ever Lived—or a Fraud?” told the story of the famed French woman, who died in 1997, supposedly at the age of 122. But when historical inconsistencies started popping up, investigators discovered that the woman who died may have been a masquerading daughter. Lauren Collins wrote, “Jeanne Calment … was an accidental icon, her celebrity the result of a form of passivity. For a hundred and twenty-two years, five months, and fourteen days, Calment managed not to die.”
But Filippa and Diega Cammalleri were real – and studied.
The anti-aging industry is one-size-fits-all
The researchers gave the sisters a detailed questionnaire in July 2017, took all sorts of measurements, and did blood and limited genetic analysis. What their findings reveal about their physiology runs counter to what the “anti-aging” industry promotes to supposedly make us live longer – in several ways.
It turns out that the super-old sisters likely lived as long as they did because of high levels of pro-oxidants and low levels of anti-oxidants, plus steady low-level inflammation. Filippa had an unhealthy cholesterol profile, and the sisters apparently shared a sweet tooth.
 “Aging” in biological terms, means “change over time.” Therefore, the only anti-aging strategy is to cease being alive, or to take a ride in a time machine. However, as is clear during this time of the pandemic, popular ideas don’t always make scientific sense.
“Aging” in biological terms, means “change over time.” Therefore, the only anti-aging strategy is to cease being alive, or to take a ride in a time machine. However, as is clear during this time of the pandemic, popular ideas don’t always make scientific sense.
Consider Sephora, the chain of product-packed cosmetics and skin care superstores. Their anti-aging elixirs include peels, serums, polypeptide moisturizers, oils, the utterly useless collagen (too large a molecule to get under skin) pitera essence (a “miracle ingredient” from sake; as soon as I googled it Facebook tried to sell it to me), lactic acid, retinol cream, leechee nuts, hyaluronic acid, and of course the ever-present anti-oxidants.
Questions and measurements
The sisters lived all their lives in Canicattì, Sicily. What made them tick for so long?
They answered wide-ranging questions. What had made each sister sick? Which drugs had they taken? Did they smoke? Tests assessed depression, cognitive status, activities of daily living, ability to perform complex tasks, and sleeping and eating habits. I didn’t see a mention of exercise.
Metrics included body mass index and bioelectrical impedance analysis. “BIA” measure fat versus lean muscle mass through a weak electric current passed through the back of a hand and a foot.
The family history was straightforward, revealing longevity and colon cancer.
Filippa and Diega’s father Calogero Cammalleri died at 97 of unknown causes, and their mother Maria Di Pasquale died at age of 73 of the cancer. Twin sons died of colon cancer and a third son in an accident.
Diega taught at a primary school; Filippa went as far as fifth grade. The sisters never married and lived together in an apartment. They were wealthy enough to afford a live-in caregiver.
The sisters never smoked, slept 5 to 6 hours a night, and took anti-hypertensive drugs, diuretics, and antiplatelet agents. Diega had macular degeneration and Filippa had cataracts. Both suffered from arthrosis (a breakdown of joint cartilage without inflammation) and osteoporosis.
Filippa was hospitalized at age 100 for a broken femur and five years later for constipation. She had mild dementia. So their medical histories were unremarkable.

Only for their final decade had the sisters needed help with dressing, hygiene, going to the bathroom, getting around, and eating. During those final 10 years they also couldn’t prepare meals, take care of their finances, do the housekeeping, use the phone, and manage their medications.
As for eating habits, the Cammalleri sisters didn’t stick to the much-praised Mediterranean diet. They enjoyed pasta, extra virgin olive oil, milk, and fruits, but only ate vegetables two or three times a week. The sisters consumed pastries and/or biscuits twice a day, eggs and potatoes once. They ate red or cured meat once or twice a month, but liked white meat chicken and bluefish. The investigators deemed their diet of mostly legumes “monotonous.”
Delving into the data
The sisters were small and thin, technically sufficiently so for the word “cachexia” to appear: “wasting syndrome.” Each woman was a little over 5 feet tall, Filippa weighing 110 pounds and Diega 117. One of the physiological tests (for PhA, aka polyhydroxyalkanoate) attributes their small bodies to fluids leaking out of their cells.
I analyzed the four tables of test results to see if my interpretation matched the researchers’ conclusions. And it did.
The tables list:
- Anthropometric and body composition values
- Blood tests
- Oxidative and inflammatory tests
- Limited genetic tests (a few genes and microRNAs)
The tables are a nice visual way to present the findings. Each has four columns. Leftmost is the test, then a column for each sister, then a column for normal range for the metric in healthy Italian women aged 50 to 65. Boldface indicates where each sister is out of range, so thankfully I didn’t need to deal with any actual math.
Only a few boldface measurements appeared for all entries except for “oxidative and inflammatory tests.” Of those dozen markers, the twins were literally off the charts.

Paradoxical anti-oxidant patterns and microRNAs spell inflammation
The sisters had low levels of anti-oxidants, such as PON (paraoxonase) and GSH (glutathione), and of the sulfur-containing amino acids needed to make them. Yet they had high levels of MDA (malondialdehyde), a marker for oxidative stress. Elevated KYN (kynurenine) reflected body-wide inflammation, which is part of the innate immune response.
The findings for microRNAs were telling too. MicroRNAs are tiny RNA molecules that flit on and off different combinations of genes, blocking some of them from being transcribed and translated into protein. They’re described as “dimmer switches” for the genome. Combinations of the 2,500 or so microRNAs in the human genome oversee and fine-tune protein production.
The levels of three types of microRNAs circulating in the sisters’ bloodstreams conferred what the researchers call a “longevity phenotype” – a level of inflammation normal for a much younger person.
Was an immune system allowed to simmer on a low burn responsible for a long lifetime without infectious disease?
Limited genetic info
The genetic analysis was just a few markers of aging, not a genome-wide landscape of single-base (SNP) markers, or an exome or genome sequence.
The researchers considered two genes associated with aging: FOXO3A and ApoE.
At one place in Forkhead box O3A (FOXO3A), a person can have two DNA bases of “GG,” two of “TT,” or one of each, “TG.” Having a “G” has been linked to longevity. Filippa was TG and Diega TT. It turns out that the association holds for just some populations, Sicilians not among them.
The ε2, ε3, and ε4 variants of the ApoE gene were also on the menu. This gene is widely known for its association with Alzheimer’s disease risk: the ε4 variant raises risk, ε2 lowers it, and the most common ε3 variant is neutral. The sisters had boring ε3 variants. Again, the genetic associations don’t hold for Sicilians.
Returning to metabolism for a moment because it’s under genetic control, the sisters had borderline unhealthy cholesterol profiles. Diega had low HDL and Filippa had low HDL and also high LDL.
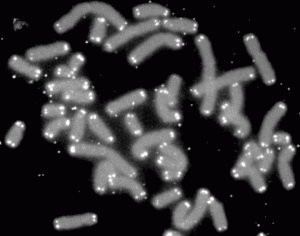 Telomeres were measured. These are the chromosome tips that normally whittle down with age. Longer telomeres might be expected in people who live a long time, but the sisters were again normal.
Telomeres were measured. These are the chromosome tips that normally whittle down with age. Longer telomeres might be expected in people who live a long time, but the sisters were again normal.
There’s precedent for the finding that low-level inflammation keeps some folks alive for a long time. A 2015 paper, “Inflammation, But Not Telomere Length, Predicts Successful Ageing at Extreme Old Age: A Longitudinal Study of Semi-supercentenarians,” from researchers at the Centre for Supercentenarian Research, Keio University School of Medicine, in Tokyo, found this to be a commonality among most of the 1,554 very old folks they analyzed.
“We conclude that inflammation is an important malleable driver of ageing up to extreme old age in humans,” they wrote.
What does it mean?
The two sisters who surpassed their 100th birthdays in relatively good health had:
- Elevated LDL cholesterol
- Modest, persistent inflammation
- Oxidative stress
- Twice-a-day consumption of sweets
- Limited veggies
- No protective ApoE genes against Alzheimer’s
Diega and Filippa are clearly exceptional. But they do make the case that one-size-fits-all medicine isn’t always the best way to evaluate health. Journal articles applaud precision medicine, but the average health care consumer is unlikely to encounter it.
My primary care provider has never asked me a single thing about my family health history. If she had she’d learn that there’s no cardiovascular disease at all, yet unhealthy cholesterol profiles. She wants me on a statin. Well, no. She keeps prescribing naproxen, even though it makes me sick, because insurance companies and protocols recommend it be given first because ibuprofen irritates the digestive lining. But ibuprofen does that in only one percent of the population, and that’s not me.
Diega and Filippa were lucky – we don’t know whether they actively did anything to prolong their lives. But the subtext to studying biologically exceptional people is that we learn more about how we vary. And health care providers should consider that their patients could be exceptions to medical rules.
Ricki Lewis has a PhD in genetics and is the author of the textbook Human Genetics: Concepts and Applications, soon to be published in its fourteenth edition. Follow her at her website www.rickilewis.com or X @rickilewis
A version of this article was originally published at Plos Blogs and has been republished here with permission. PLOS can be found on X @PLOS
This article first appeared on the GLP June 5, 2023.































