Diffusion Tensor Imaging (DTI) an ambiguous biomarker of brain injury
An advanced MRI technique, known as diffusion tensor imaging (DTI), is used as an indirect indicator of white matter structural integrity. This technique measures the diffusion of water molecules in the brain’s axons. To generalize, the MRI measures the movement of water molecules. The flow rate is faster along linear, unimpeded pathways, and less so as these pathways twist and turn. The accuracy of DTI is severely limited when paths are crossing one another. Various DTI parameters are measured throughout the brain, with names such as “axial diffusivity” and “fractional anisotropy.” It is well-established that these DTI parameters change following a traumatic brain injury in humans, and experimental animal research confirms that cellular injury is responsible for this. Based on this information alone, it may seem reasonable to claim that the brain’s structural integrity remains unchanged if the DTI parameters remain constant. Unfortunately, this is a classic example of the inappropriate oversimplification of biomarker analysis.
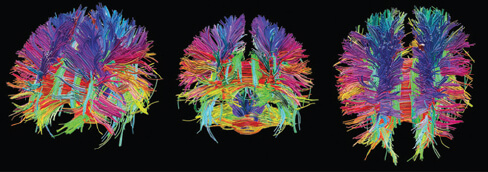
Another inherent issue here is that one must assume that stable DTI parameters are normal and desirable when scientific research suggests otherwise. Plenty of research has demonstrated the brains of adolescents typically experience DTI parameter changes with maturation – it should not be surprising that growing brains are experiencing structural changes. Likewise, physical and non-physical training also influences changes in DTI parameters. Perhaps most importantly, animal research has demonstrated that DTI parameters may eventually return to normal after brain trauma, even though biopsy data reveals damage persists within the brain tissue.
Brain imaging biomarkers, such as DTI, involve multiple parameters with highly variable responses, across a large number of the brain’s anatomic regions. With so many measurements, it is quite likely that “significant” results could be identified by chance alone, especially when statistical techniques to account for multiple comparison corrections are not performed. Bennet and Baird eloquently demonstrated this with functional MRI data, as they found statistically significant signals associated with emotional responses to various stimuli could be detected on a dead salmon when appropriate statistical corrections were not utilized.
Science meets the marketplace
Some companies use biomarker data from human clinical trials to justify scientific-sounding marketing claims that their product is effective in “protecting the brain.” Though complex analyses published in peer-review journals may superficially suggest product effectiveness, critical analysis reveals that interpretation of biomarker data is far too nuanced and biased to demonstrate evidence of “brain protection.”
One device which has received considerable attention from the mainstream media is a collar that mildly compresses the jugular vein. According to product stakeholders, this creates a small backflow of blood, which ultimately cushions the brain and reduces how much it sloshes around inside the skull after an impact. Supposedly, this device mimics the natural physiology that woodpeckers use to protect their brains, but a thorough review of the scientific literature indicates that woodpeckers have no such mechanism.
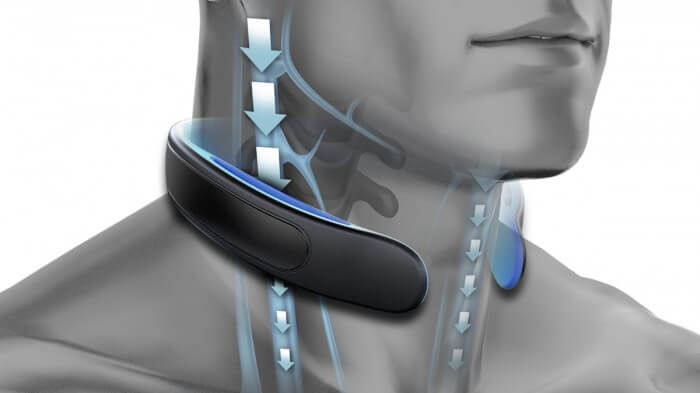
In the case of the jugular compression collar, changes in DTI parameters throughout a high school sports season in those not wearing the device have been interpreted as evidence of structural changes in the brain, and those changes are presumed to be detrimental. Thus, the lack of change in DTI parameters in those using the device is seen as evidence of a “protective effect.” Closer examination reveals that the DTI parameters within any given individual wearing a jugular collar does not actually stay constant at pre-season levels, but rather increases or decreases after a season of play. Thus, the different directions of DTI parameter changes cancel each other out, and those wearing the device spuriously appear to have statistically unchanged DTI parameters. This group-level mathematical artifact is certainly not evidence of an individual-level protective effect!
Thus, the significant changes in DTI parameters in those athletes not wearing a collar are not necessarily pathologic. Instead, they could simply represent normal growth and development and participation in sports or recreational activities (regardless of head impact). Conversely, “stable” DTI parameters following use of a jugular compression collar may not actually indicate “brain protection,” but rather an aberration from normal adolescent development. The notion that jugular compression yields a different trajectory of DTI parameters is especially concerning, given recent animal experiments that suggest jugular occlusion actually impairs our brain’s normal waste removal system (the “glymphatic system”) and that this may exacerbate traumatic brain injuries. As mentioned earlier, the issue of false-positive results from numerous statistical comparisons must also be considered, given inconsistent reporting between the various studies examining jugular compression.
Nevertheless, marketing materials cite MRI data indicating that wearing this device protects the brain’s white matter structural integrity after exposure to sports-related head impacts. Seeing a minimal change in DTI parameters following regular use of a “protective” device tells us very little about lasting brain damage and long-term brain health. Thus, DTI data do not provide us any real insight into whether or not a product “protects the brain.”
What are the consequences of overselling current brain biomarkers?
As new products emerge with scientific-sounding data, they will likely be adopted by athletes and sports organizations as a “quick fix” to address the concussion crisis. When weak biomarker data is extrapolated into “proof” that a commercially-available product protects the brain, it gives athletes and other stakeholders a false sense of safety and diverts attention from more reasonable injury-prevention strategies. Parents may allow their children to participate in more dangerous sports, and athletes may engage in riskier behavior on the field – a concept known as risk compensation. This is especially dangerous if the intervention of interest does not provide any actual protective effect. Athletes will continue to get exposed to head impacts. Regardless of how our current biomarkers change with these traumatic events, we will not know until years or decades after the long-term damage has happened.
James Smoliga, DVM, PhD, FACSM is a Professor of Physiology in the Department of Physical Therapy at High Point University. He earned his Doctor of Veterinary Medicine from Cornell University, before completing his PhD in Sports Medicine at the University of Pittsburgh. His research interests include sports medicine, exercise physiology, and translational medicine. Most recently, he has been working to debunk pseudoscience and improve the quality of scientific research, while taking on a greater role in scientific communication. Find James on Twitter @jsmoliga
A version of this article was originally posted at the American Council on Science and Health website and has been reposted here with permission. The American Council on Science and Health can be found on Twitter @ACSHorg































