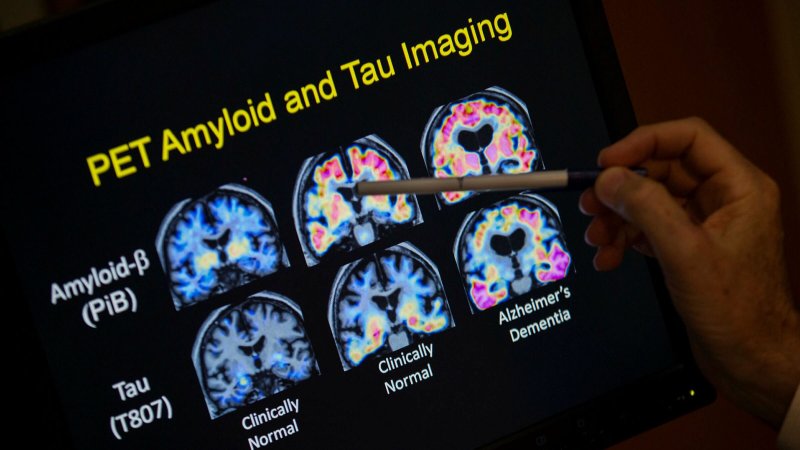
Alzheimer’s disease was to be defined by the presence of plaques. Yet plaques are a feature that is not present in 15 percent of the people with a clinical diagnosis of Alzheimer’s, and a feature that is present in people of all ages including 30 percent of elderly people without any cognitive impairment. If this doesn’t make sense to you, it’s because it doesn’t make sense.
In the basic research laboratories of the world, data kept accumulating that violated the expectations of an amyloid-only definition for Alzheimer’s disease biology.
In response the NIA began to recognize that there was a “broad consensus … that the criteria should be revised to incorporate state-of-the-art scientific knowledge.”
The result was a truly comprehensive review — a compendium of four papers comprising reports of three working groups plus an introductory summary.
Coming as it did, a full quarter century after the Consortium to Establish a Registry for Alzheimer’s Disease (CERAD) working group met, it would have been an ideal platform to announce the decision to cut the definition of Alzheimer’s disease loose from the presence of plaques.
Instead the experts in the field doubled down and bet the store on amyloid. In doing so, they made the entire situation much, much worse.