Eric J. Topol, MD: Hello. I’m Eric Topol, editor-in-chief of Medscape. It’s a special privilege for me to welcome Paul Offit [director of the Vaccine Education Center at Children’s Hospital of Philadelphia], who is my go-to expert on vaccines. It’s an opportune time to talk about the vaccine for COVID-19. Paul, welcome.
Paul A. Offit, MD: Thank you, Eric.

Topol: This is a really critical juncture for the vaccine against SARS-CoV-2. I know you’ve been intimately involved with this for quite some time — well before there was a pandemic, and now that we’re in the midst of it.
Before we get into some of the nitty-gritty, can you just give us your overall view of the landscape on this?
Offit: Well, it’s an unprecedented moment. Never before in history have so many companies, or so much money, or so many different ideas for how to make a vaccine been brought to play. We’re using every strategy that has ever been used to make a vaccine before, as well as a handful of strategies that have never before been used to make a vaccine.
It’s all happening at warp speed, and at some level, that’s disconcerting. A lot of the language that surrounds this — “warp speed,” “finalist,” “race for a vaccine” — scares people that either timelines are being inappropriately truncated or, worse, that safety guidelines are being ignored.
But I think that we’re good. Right now, eight companies are in the midst of phase 3 trials — large, prospective, placebo-controlled trials — to prove efficacy, at least for a certain length of time, and to prove safety, at least in a certain number of people.
As long as the phase 3 trials don’t get truncated, we’re okay. And as long as the Trump administration doesn’t try to reach its hand into Warp Speed and pull out a couple of vaccines and oversell them — because there aren’t enough data yet — I think we’re fine.
Topol: Before we get into that, there are several different types of vaccines being tested. The two that the US has put its biggest bets on are the mRNA vaccines from Moderna and Pfizer. But obviously there are several other vaccines, eight that are in phase 3 trials.
What’s your sense about the mRNA vaccines? They have never been used in people before in a vaccination program, whereas the other approaches, at least some of the others, have. Do you think there is any worry about having a genetic vaccine?
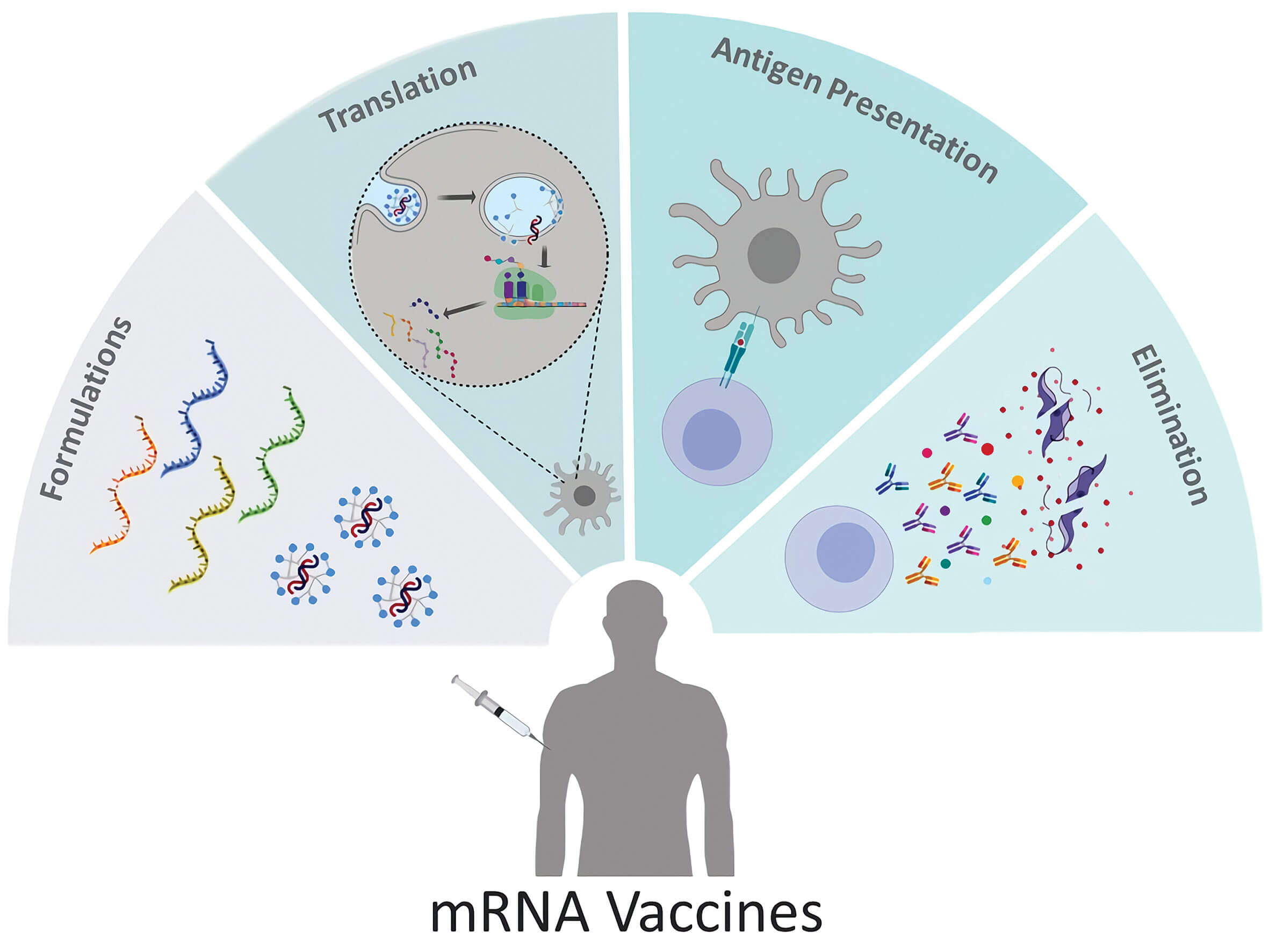
Offit: I think when you have no commercial experience with a vaccine strategy and you’re using that as a way to try to stop a new virus, there will be something of a learning curve. In addition, this bat coronavirus, which has just made its debut in the human population, has had a number of surprises, clinically and pathologically.
No one would have expected that an enveloped respiratory virus that is spread by small droplets would rage in a hot and humid climate during the summer, a time when the flu is gone. No one would have predicted that it would cause this unusual multi-inflammatory syndrome in children; I know of no other virus that does that.
I think the most surprising aspect of this virus is that it causes vasculitis, but not because it reproduces itself in the endothelial cells that line blood vessels. I think the vasculitis is a function of the immune response, and a panel of cytokines and chemokines are causing that. As a consequence, you can have strokes, heart attacks, liver, kidney, and other distal organ disease.
It also seems to have a predilection for nursing homes. Influenza also kills older people, but fewer than 10% of influenza deaths are in nursing homes. Here, it’s more than 40%.
So you have this difficult-to-characterize, elusive virus that you are now about to meet with a handful of vaccine strategies for which you have no commercial experience. I think you can assume that there may be a learning curve here.
I wish there was a little more humility from some of these companies. They’re always sort of pounding their chests as to how they’re going to have this vaccine. I think, just in the past day, the CEO of Pfizer said, “I think we can have a vaccine by the end of October.” I’m sorry; are you on the Data Safety Monitoring Board (DSMB)?
Topol: We want to get into the DSMB, and the advisory board, and some of these really critical decisions that are coming up at the end of October — before November 3, that is.
But before we do that, I want to go back a little bit to the biology you just touched on. We have tropism of the virus to many places in the body, wherever there is ACE-2 expression. We also have this immune inflammatory response to that. So it’s hard to separate the two, as you mentioned.
The virus can get into endothelial cells, but there is also the inflammatory and cytokine reaction to that entry. The same as in the heart, as in the kidney, the brain. This is a really tough nut to crack.
Moreover, there are a lot of things that we still don’t understand. Like, for example, “long COVID.” What is your sense about long COVID?
Offit: You’re referring to people reporting long-lasting symptoms, such as depression, joint pain, low-grade fever?
Topol: Right. Joint pain, brain fog, chest discomfort, difficulty breathing, very poor exercise tolerance, some that has been continuing since acute infections in March. For some people, it is still going on and very disabling. But it seems to affect an unknown percent of people.
Offit: I think it’s probably a reflection of a couple of things. In part it is probably because of the vasculitis which is causing damage in a variety of organs, and that can be chronic. Scarring of the lung can be somewhat disabling. I think we’ll learn about that over time.
Then there may be an ICU psychosis associated with this; for patients who are in the ICU for a long time, when they come out of it, there’s a sort of brain fog, or depression, which may be part of this. So I think there may be overlapping things going on.
I think it’s real. I don’t think it’s just something people are making up. I think this is a real problem. We’ll learn about it as we gather more information on this virus.
Vaccine Trials Take Time
Topol: Turning to the vaccine. There are the two 30,000-participant, placebo-controlled trials with the Pfizer and Moderna vaccine candidates, which are expected to complete enrollment by end of this month.
Both of these have a two-dose program. So after the first dose, there’s a booster a month later, and then it will take a few weeks before you’d see the full expected immune response.
Knowing that enrollment will only finish this month at best, can you explain how we could have a readout of these two phase 3 trials by the end of October?
Offit: I don’t see how it’s possible. Moncef Slaoui, who’s the head of Warp Speed, has, I think appropriately, said recently on a National Public Radio show that he thought a best-case scenario would be the end of the year, most likely the beginning of next year. I think that’s a more accurate representation.

As you said, you have to get 30,000 people to get dose 1 of placebo or vaccine. You have to wait a month, give 30,000 people dose 2 of placebo or vaccine, wait 2 weeks to full immunity, then you have to hope that about 150 or 160 people in your placebo group get sick. Not just infected, but sick. The clinical endpoint in these trials is moderate to severe disease.
Jackie Miller from Moderna presented to the Advisory Committee on Immunization Practices (ACIP) last week and was asked what the attack rate is in the places where they’re rolling out these trials. They’re getting antibody studies on all of the people when they enroll so they have a sense of what the attack rate has been. It’s about 1%.
If that’s true, and remembering that 80% of the disease is asymptomatic, you’re focused on the 20% that’s symptomatic in an area where only about 1% of people have been infected. And you’re also telling people to wear a mask and social distance, because one, they may be placebo recipients, and two, no vaccine is going to be 100% effective. In many ways, you don’t want them to get sick, but on the other hand, you’re only going to know if the vaccine works if a certain number of them get sick. You’re not asking them all to go to Sturgis, South Dakota, and hang out with a mess of bikers. You want them to be protected at some level.
Topol: Do you know if the two programs are enrolling in Brazil in high zones of infection and spread? Has that attack rate been published anywhere?
Offit: We know it from conferences. The trials are being done in the United States, South America, Africa, in areas that presumably are hot so it increases the chance you’ll be able to get a representative number of clinically significant illnesses in your placebo group.
But again, even in the best-case scenario, I can’t imagine that happens before the end of the year, assuming that our goal here is the same as it is for every vaccine, which is a clear standard of safety and efficacy for any licensed vaccine.
Ultimately It’s Up to the Companies
Topol: There’s a DSMB for each of these phase 3 trials, which is a multidisciplinary group, including people who are experienced with clinical trials, biostatisticians, bioethicists, immunologists, vaccinologists, and virologists. You have this big crew, they’re reviewing the blinded data, and they have a pre-programmed time of review. Also, they have stopping rules that are defined ahead of time for both futility and for overwhelming efficacy.
But this week, for example, the Pfizer CEO said they could demonstrate efficacy with very small numbers of cases in the placebo and vaccine groups; these numbers seem totally out of line with what would be considered stopping rules.
I mean, you’re talking about giving a vaccine with any of these programs to tens of millions of people. And you’re going to base that on 100 events?
Offit: The NIH ACTIV group was put together by Francis Collins to try to construct how these trials should look. There was a statistician from the University of Washington who went through those data. His analysis showed that you’d probably need at least 150 or 160 people in your placebo group to start to say that you have a statistically significant observation, assuming that you have just a handful or fewer people in your vaccine group who were ill.
I’d like to think that’s what the stopping rules are. That the stopping rule isn’t that you have 10 people who are sick in your placebo group and two in your vaccine group, which are numbers that are far too small to make any statements about statistical significance.
Topol: Well, the CEO of Pfizer actually was citing fewer than 100 total events, with a 50% reduction in the vaccine group vs the placebo group. To me, even 160 seems like a really small number for a stopping rule when the stakes here are so big, right?
Offit: I think one could only imagine stopping with 160 cases if you have virtually no cases in your vaccine group.
Topol: And to clarify, because this is important, we’re not talking about just a PCR-positive mild infection. It has to be moderate to severe illness to qualify as an event, correct?
Offit: That’s right.
Topol: Now, the other part about this story is that the DSMB isn’t supposed to be reporting to the company. It’s supposed to be reporting to the trialists who are testing the vaccine. How independent are these academicians?
Offit: Historically, the DSMB reports to the company. They go to the company and say, “We are at a point now where you could argue, statistically, that you have efficacy.” The company then has the option, if they want, to stop the trial. But that isn’t common.
Topol: That is interesting, because in the trials I’ve been involved in, the company was out of the loop. And only after the trialists reviewed the DSMB information was there was potential discussion with the company. This is an interesting difference.
Now let’s talk about the committee that you’re on, which is the FDA Advisory Committee, right? That’s the committee that’s meeting October 22 that has been called out by the FDA commissioner, saying that he doesn’t have to honor the recommendation. He can override that if he wants. Can you tell us about your committee?
Offit: Like the DSMB, it is independent of the government, it is independent of the company. It’s academicians looking at data and making recommendations. The same thing is true of the FDA vaccine advisory. It’s independent of the government and the companies. We’re paid by neither; we’re just academicians.
But like the ACIP to the CDC, the FDA’s vaccine advisory committee gives advice. We can say, “I think that this vaccine or these vaccines are not ready to be given to the American public.” The FDA commissioner and his team then have the ability to either take that advice or not take that advice. They can always ignore it.
I think that would be hard to do, though The public is seeing this meeting at the same time that we’re having the meeting. And if you have people saying, “I don’t think we’re there yet. I wouldn’t get this vaccine” — with an already skittish American public, I think they would defeat themselves by ignoring that.
Topol: Yeah, you’re talking rationally now, which is good; that’s refreshing. The point is that we’re not going to have a phase 3 trial completed by October 22. The only way it could be completed is if there was some stopping rule that allowed someone to make the call by October 22, which seems virtually impossible, based on what we know.
That means that the data discussed at your October 22 meeting are going to be based on a midstream, still-blinded, ongoing trial, right?
Offit: Unless the code is broken by the DSMB — broken because they think that they’ve met a standard for efficacy and safety — we won’t see those data.
The only way we would see those data is if the DSMB said, “I think we’re good.” And then it would go to the company, because the company is the one who ultimately puts that vaccine out there. Ultimately it is their reputation when the vaccine is put out there. I would like to believe that there is no interest in the company putting a vaccine out there that’s unsafe or ineffective. Many of these companies have other vaccines, international portfolios of vaccines, and that would tarnish all of them.
Topol: There is a lot on the line.
Offit: Another option for the October meeting is we discuss what kind of data we’re looking for to comfortably recommend the vaccine. Do we want to see different subgroups recommended? People who are over 65, people who have various small comorbidities, etc. What kind of data are we looking for, because the FDA may have other meetings scheduled this year.
A Higher Standard for Vaccines
Topol: Well, that gets me to our friend Anthony (Tony) Fauci, who was on CNN recently talking about the possibility of an imminent emergency use authorization (EUA) for a vaccine prior to a phase 3 trial completion.
Tony basically said that he trusts the FDA, that they will make the right decision. My concern is that they just grandstanded about convalescent plasma, and prior to that they issued an EUA for hydroxychloroquine, which they had to revoke. And the data, obviously, hadn’t supported either of those.
Why would we have any sense of trust that the FDA won’t make the call on a vaccine before a phase 3 trial is completed? We don’t exactly have a consistent, reliable, science- and evidence-based story from the FDA since this pandemic started.
Offit: I think you’re right. Hydroxychloroquine should have never been given an EUA. There was no evidence to show that it worked. We certainly knew even early on that it could cause cardiac toxicity arrhythmias. That was a mistake, and it was withdrawn.
I feel the same way about convalescent plasma. I think that should have never been approved. I mean, those data certainly don’t support its use. Both Drs Collins and Fauci had, before that EUA was granted, said they didn’t think the information is there to support it. Since the EUA was granted, the NIH put out a paper saying they don’t think it works.
That’s two swings and misses. In both cases, those were therapeutic products given to people who were already sick. I’m choosing to believe — and I am an eternal optimist — that we will hold something that is about to be given to otherwise healthy people, many of whom are not likely to die from this virus, to a much higher standard.
Topol: Well, I like your optimism, and it’s really good to share some of that sentiment now.
We haven’t talked enough about safety, which isn’t just about the immediate reactions to the injections but rather, as people who have received the vaccines are exposed to infections over time, some may have an untoward immune response.
It could be an antibody-dependent enhancement. It could be potentially some type of immune-complex disease. Are you concerned about these other risks that have not been ascertained and are of low incidence, such that you need thousands of people to get a readout on them?
Offit: For people who are considering these issues, I think what worries them the most is a vaccine-induced immunopathology. In other words, look at the measles and RSV vaccines of the 1960s. Those were two inactivated vaccines which, when given to people, actually put them in a worse position.
Children who got this inactivated RSV vaccine were more likely, when subsequently exposed to wild-type virus, to be hospitalized with pneumonia and to die than were children who never received that vaccine. The same is true with the inactivated measles vaccine, which actually was a licensed product for a little while, and which caused atypical measles, with pneumonia and hospitalizations.
Both of those viruses have fusion proteins, which they use to fuse to the cell for entry. It’s not the typical attachment, then transport in by endocytosis. The concern was that during vaccine preparation this prefusion confirmation of the virus had been converted to the postfusion confirmation. So people were being inoculated with something that they would not normally see when they were exposed to wild-type virus.
At least the immunopathologic response in those situations was the so-called Th2 response, which is associated with a different set of cytokines from Th1 responses. People are aware of that issue. If you look at the papers that are coming out, even phase 1 studies, people are always looking at that T-helper cell response and whether it’s inducing a Th1 or Th2 response. So that’s on people’s minds.
Regarding antibody-dependent enhancement — which certainly was a problem with the dengue vaccine — instead of making neutralizing antibodies, the vaccine induces binding antibodies that help the virus enter cells, so-called antibody-dependent facilitation or enhancement. But again, people are looking at neutralizing vs binding antibodies and their longevity with that in mind.
And you’re only going to know about rare adverse events once these vaccines are out there, because even in a best-case scenario, they are tested on 20,000 or 30,000 people, not 20 million or 30 million people. So you’re only going to know about a rare adverse event post-licensure. But there are systems in place like the Vaccine Safety Datalink, which I think can pick that up. And the CDC is certainly well aware of this and has systems in place to look for this once the vaccine rolls out.
Topol: So let’s say you started giving this vaccine whenever it gets approved, likely early next year if it’s done legitimately. But there are not going to be many people in the phase 3 trials who have had prior infections, right?
Offit: Well, it’s true that they’re not being screened out for that. For the most part, everybody gets an antibody test when they enroll in one of these vaccine trials. And whether they’re positive or negative, they’re still included. So that’s good because it would be impractical to do it any other way when we roll it out.
Topol: So some people in these trials have had a prior infection.
Offit: Jackie Miller last week told ACIP that the rate was low, about 1%.
Topol: That’s very low when all the models suggest that 13%-14% of people in the United States have had infections. And those people could have a different immune response from the people who are naive to the virus. Is that a reasonable concern?
Offit: I think it’s something to keep your eyes open for. We’ll know when we look at these phase 3 trials who was antibody positive in the beginning and who wasn’t. In many ways, it’s a good thing that we’re letting those people into the trials, because that’s similar to the natural situation.
Topol: What else besides these immune-mediated or facilitated mechanisms are you concerned about, regarding safety?
Offit: With the mRNA vaccines, mRNA itself is a safe molecule. We all have mRNA in our body; it breaks down very quickly. But because it’s such a labile molecule, it is encapsulated in this complex lipid delivery system, which is reactogenic. When you inoculate people with lipids, they get fever, including occasionally high fever. And when you’re giving a fever-inducing agent, you could either trigger or exacerbate any sort of immunologic disease. So that’s one issue.
Then there are the replication-defective virus vaccines, like the replication-defective simian adenoviruses being produced by AstraZeneca. Also, there is the replication-defective Ad26, which is being pursued by Johnson & Johnson, and the replication-defective Ad5, which is being pursued by both the Russian and Chinese groups.
Here, the good news is that each of these is replication defective, which means that the virus can’t reproduce itself and cause harm. The bad news is, you really just get one cell per virus particle to make the protein you’re interested in, which is the coronavirus spike protein. So you give a lot of virus. I think the Russian paper that just came out on September 4 gave 100 billion virus particles.
You know, it was a replication-defective adenovirus that was given to Jesse Gelsinger, whose death was the first directly related to gene therapy.
Topol: I forgot that it was a defective adenovirus.
Offit: So with that you worry that you could induce a massive cytokine response, which is what happened to Jesse Gelsinger. Now we have monoclonal antibodies directed against interleukin-6, like tocilizumab. We didn’t then, so Jesse Gelsinger unfortunately died. But you always wonder when you’re giving that many viral particles whether you could trigger that sort of response.
Trial Participants Should Reflect the Broader Population
Topol: So safety is something that we won’t really know about when the trials are reporting out, let’s say in the first quarter of next year. That will be especially true given the small number of participants who’ve had prior infections, in whom you might have heightened concern for their response.
Offit: I think that is true of every medical product. You can say with some confidence that you can rule out a relatively uncommon, serious side effect in a phase 3 trial. But you can’t rule out a rare side effect. As you go from phase 1 to phase 2 to phase 3, from 20 to 100 people, to hundreds of people, to tens of thousands of people, you reduce uncertainty. But you never eliminate uncertainty.
Topol: Right, but another issue is that people in these trials are not very representative of Americans; they’re largely a White population. Underrepresented minorities are not well represented, nor are the aged or children.

Offit: I think these products cannot be recommended for someone who is greater than or equal to 65, unless there are clear safety and efficacy data in that age group. Similarly, I think that if we’re going to be giving them to people who have certain comorbidities, one of the most common of which would be obesity, then you would like to see that those people are adequately represented in these trials.
Children are not going to be in the initial trials; everybody in these initial trials is greater than 18 years old. So I’m certain that these vaccines are going to start to roll out before we’ve ever tested them in children. Then the question becomes, how do you test them in children when you have products which have been approved and shown to work?
It’s hard to do placebo-controlled trials when you know you have a vaccine that works. So I imagine the way that would play out would be as a wedge trial — the same way that the Ebola vaccines played out in West Africa — which is, you start to give the vaccine, knowing that you’re not giving it to everybody all at once.
In that case, you can see the efficacy and safety by comparing those who received it with those who didn’t. It’s not a prospective, placebo-controlled trial, which means you have some confounding variables, but I think that’s the way that would likely play out.
Topol: So the highest-risk people, or among the highest-risk people, are those over age 65, and we aren’t going to have data that are sufficient to address that group at the end of phase 3?
Offit: If we don’t have adequate data in the greater-than-65-year-old group, then the greater-than-65-year-old person shouldn’t get this vaccine, which would be a shame because they’re the ones who are most likely to die from this infection. We have to generate those data.
I can’t see how anybody — the DSMB or the FDA Vaccine Advisory Committee, or FDA decision-makers — would ever allow a vaccine to be recommended for that group without having adequate data.
I feel the same way about minorities. I mean, you can’t convince minority populations to get this vaccine unless they are represented in these trials. Otherwise, they’re going to feel like they’re guinea pigs, and understandably so.
Building Public Trust
Topol: Well, that gets us to the public trust and the fact that willingness to have the vaccine is important. Because if there is terrible mistrust, we won’t ever get to the level of immunity in the population.
Offit: It’s hard to promote trust now absent data. Once we know the characteristics of these vaccines, it’ll be much easier to try to explain what we know and what we don’t know. Because I really do think it’s going to be a matter of managing expectations.
Let’s say we have a vaccine that is theoretically 75% effective against moderate to severe disease, and we know that it’s been given to 20,000 people and that your group has been represented. And let’s assume that the virus is still killing 1000 people a day and causing people to be hospitalized and suffering. It’s never a matter of when you know everything. The question is, when do you know enough? When do you know enough to say that a vaccine’s benefits outweigh its theoretical risks?
You have to also make sure people know what you don’t know. You don’t know how long protection is going to last. You’re only going to know that afterwards. You don’t know whether it causes a rare side effect. You’re only going to know that afterwards. But there are systems in place to find out both of those things. I just think we have to be honest and transparent about what we know and what we don’t know.
Managing Expectations
Topol: We’ve covered a lot, Paul. Have we missed anything important?
Offit: I’ll tell you the thing that keeps me up at night on this particular issue. We have two ways of stopping this virus: One is hygienic measures — face masks, social distancing, handwashing — and the other is the vaccine. With those two, we will be able to bring this virus under control. But it will take both.
What worries me is that if you had to pick which is the stronger of the two, I would go with hygienic measures. I mean, if I wear a mask and stand 6 feet away from you, and you wear a mask and stand 6 feet away from me, the chances that I’m going to get the virus from you or you from me is about zero. You have two things going for you. One, you have a mask, which is going to prohibit the virus’ small droplets from traveling very far. And two, even if I didn’t wear a mask and stand 6 feet away, the odds are also that you wouldn’t get it.
Topol: And by the way, if you do get it, you get a lower dose of virus, which is important.
Offit: That’s right. You might get more mild disease.
On the other hand, if we have a vaccine and it’s 75% effective against moderate to severe disease, that means 1 out of every 4 people can still get sick, including very sick. It also means probably a larger percentage than that 25% could get mild infection, or asymptomatic infection, which they could still shed, even to the point of contagiousness.
We’ve been asking these trials to look not only at whether they’re protecting against moderate to severe disease, but to what extent they are protecting against shed. I think that is important to know. But people have such an unrealistic expectation of these vaccines that they see it as the panacea, as the magic bullet to make it all go away.
If people have unrealistic expectations, such that they think “I’ve gotten the vaccine, I’m good. I don’t need to wear a mask. I don’t need to social distance. I can engage in high-risk activities,” then we’ve lost one of the important arms to bring this virus under control, arguably a more important arm. If, when we bring the vaccine up in terms of users, we move social distancing and masking down, we could end up having a sort of break-even effect.
Topol: Well, you’re bringing up a critical point and that is, the vaccine effect could actually increase the number of people who are asymptomatic carriers. Because they basically have protection from beyond their mucosa.
But they still have the virus in their nose and their upper respiratory tract to spread. And that’s why this coupling of continued hygiene- — masks, distance, and these other measures — is going to be important all the way through until we get a very dense immunity of the population, right?
Offit: There is a formula for this, actually. If you have a 75% effective vaccine against significant shedding, then you would need to immunize about two thirds of the American population to get the R0 to less than 1, meaning to stop spread, which is what you want.
Because you’re talking about two-dose vaccines — at least the ones that are initially rolling out — then you’re talking about 400 million doses. We’re not going to have that, obviously, when the vaccines initially roll out.
Topol: Those are very practical points. Well, I don’t want you to lose any more sleep. I’m losing a lot of sleep these days.
Paul, it’s been a real pleasure to talk to you. I’m going to check in with you again sometime in October to get an update, because a lot is going on and it’s hard to keep up with. For years, you’ve been the person I look to the most to give us a readout on what the reality is and to separate out the hype. Thank you so much, Paul. I really appreciate it.
Offit: My pleasure.
Eric J. Topol, MD, the editor-in-chief of Medscape, is one of the top 10 most cited researchers in medicine and frequently writes about technology in healthcare, including in his latest book, Deep Medicine: How Artificial Intelligence Can Make Healthcare Human Again. Find Eric on Twitter @EricTopol
Paul A. Offit, MD, is the director of the Vaccine Education Center at Children’s Hospital of Philadelphia and the Maurice R. Hilleman Professor of Vaccinology at the Perelman School of Medicine at the University of Pennsylvania. An internationally recognized expert in virology and immunology, he has published more than 150 papers in medical and scientific journals, and is the co-inventor of the rotavirus vaccine RotaTeq. Find Paul on Twitter @DrPaulOffit
A version of this article was originally posted at Medscape and has been reposted here with permission. Medscape can be found on Twitter @Medscape










































