Tell that to Dave Brethauer, a performance coach in Chicago, who told Genetic Literacy Project that he spent the better part of his adult life “fighting to find” himself following the trauma he experienced as a child. “From the time I was five till 14 I had an abusive stepdad in my life,” he said.
To cope, he found himself turning to alcohol, sex, overeating, and exercise addictions – anything to steer his mind away from the memories and pain that haunted him. He contemplated suicide, spent “time on a locked psych ward,” sought help at an addiction clinic, and was diagnosed with type 2 diabetes 10 years ago, at the age of 50. Only in the past decade has Brethauer been able to approach what he refers to on his website as an “optimal life.”
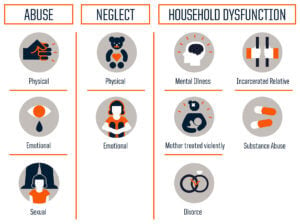
Statements about kids and resiliency are far from true, if considered in the context in which they are normally uttered: when an adult dismisses the idea that a child might be harmed by a traumatizing situation. The situation is justified or allowed to continue in light of the supposed ability of the child to handle whatever life deals them. The child might seem fine, but the effects of living through trauma are carried in their bodies and minds for a lifetime.
Kathleen Audet, image consultant in Reno, Nevada, also has trouble accepting the myth that kids bounce back. Immediately following the birth of her daughter and while still in the hospital, Audet suffered a debilitating stroke. She was only 33, and both she and her doctors knew the stroke was linked to the adverse experiences she faced as a child. “Bottom line, I was NOT listening to myself or my body,” she told GLP.
“Not listening to myself for years on end made my body shut down and say: ‘If you won’t listen to me, I’ll stop you until you do’,” Audet wrote in a post recounting her stroke and subsequent long road to recovery.
Individuals with histories of physical, sexual, or emotional abuse, or neglect “are often chronically disconnected from their bodies,” wrote Lisa Ferentz, a clinical social worker and psychotherapist, in her Psychology Today blog, entitled Healing Trauma’s Wounds. This chronic disconnection can lead to an inability to respond to normal physical sensations, like hunger and fatigue. It may also manifest as an inability or unwillingness to respond to the body’s signals that something is wrong. Disengaging from the body, Ferentz said, can become “a form of self-punishment and can set clients up for acts of self-harm” and self-destructive behaviors.
The kids are not alright
According to a large and ever-growing body of research, childhood trauma exists in all walks of life and many experts believe it is the most pressing health crisis of our time.
What we must understand is that “adversity in childhood kills you as an adult,” said Robert W. Blum, senior professor at Johns Hopkins Bloomberg School of Public Health, in a Health Happens Here video. Those who have experienced six or more traumatic events in childhood may die an average of 20 years earlier than those who have not experienced traumatic events in childhood, according to research by the Centers for Disease Control and Prevention. With appropriate treatment, however, this disparity in life expectancy could be resolved.
Children may appear unfazed or oblivious in the face of trauma because they tend to respond differently than adults. Their responses may be subtle and hard to detect, or they may be confused with behaviors coinciding with normal stages of childhood – such as increased moodiness or temper tantrums. Some children may develop self-harming or obsessive compulsive behaviors that are mostly kept hidden from parents and caregivers. They may also develop symptoms such as unexplained headaches and stomach pains, and they may get sick more frequently than their peers.
Recent research has linked childhood adversity to the diagnosis of Attention-Deficit/Hyperactivity Disorder (ADHD). Researchers from the Department of Pediatrics at the Albert Einstein College of Medicine and Children’s Hospital at Montefiore wrote in the Academic Pediatrics medical journal that children with ADHD have higher exposure to adverse childhood events “compared with children without ADHD,” and that all efforts “to improve ADHD assessment and management should consider routinely evaluating for ACEs (Adverse Childhood Experiences).” Indeed, several of the states with the highest documented rates of childhood adversity also have the highest prevalence of ADHD diagnosis.
Kelsey Torgerson, a licensed clinical social worker at Compassionate Counseling St. Louis, told GLP that “children who have experienced trauma and traumatic stress have a less developed prefrontal cortex, meaning that the part of the brain in charge of rational thinking is unable to grow.” This can manifest in the classroom, for example, as “trouble following directions, poor impulse control, and poor emotional regulation,” – symptoms and behaviors that are frequently carried into adulthood.
Children are more vulnerable to trauma than adults, according to psychiatrist Bruce Perry. In his book, entitled The Boy Who Was Raised as a Dog: And Other Stories from a Child Psychiatrist’s Notebook, Perry writes:
The developing brain is most malleable and most sensitive to experience—both good and bad—early in life. (This is why we so easily and rapidly learn language, social nuance, motor skills and dozens of other things in childhood, and why we speak of ‘formative’ experiences.) … Consequently, we are also rapidly and easily transformed by trauma when we are young.
Ever since the landmark Adverse Childhood Experiences (ACE) Study from the 1990s shed light on the long-lasting psychological and physical effects of childhood trauma, more work has been done to tease out the specifics of the connections between traumatic early experiences and the development of chronic diseases and disorders later on.
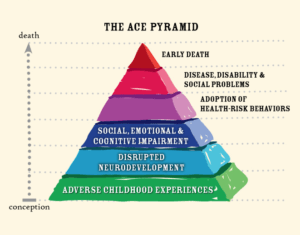
Individuals with a history of childhood trauma are more likely to develop the most common conditions associated with disability, chronic pain, and early death. These include ischemic heart disease, cancer, stroke, chronic lung disease (like asthma, recurrent bronchitis, and COPD), diabetes, liver disease, autoimmune diseases, obesity, sleep disturbances, and psychiatric disorders.
The chief mechanism behind the increased incidence of medical and psychological problems in those with high ACE scores could be linked to epigenetic changes.
There are a few theories about how epigenetic changes could ultimately result in poor health outcomes. One leading theory is represented in the following illustration, which highlights the cascade of events – including a weakened immune system and altered behavior/psychological changes – resulting from the epigenetic shift:
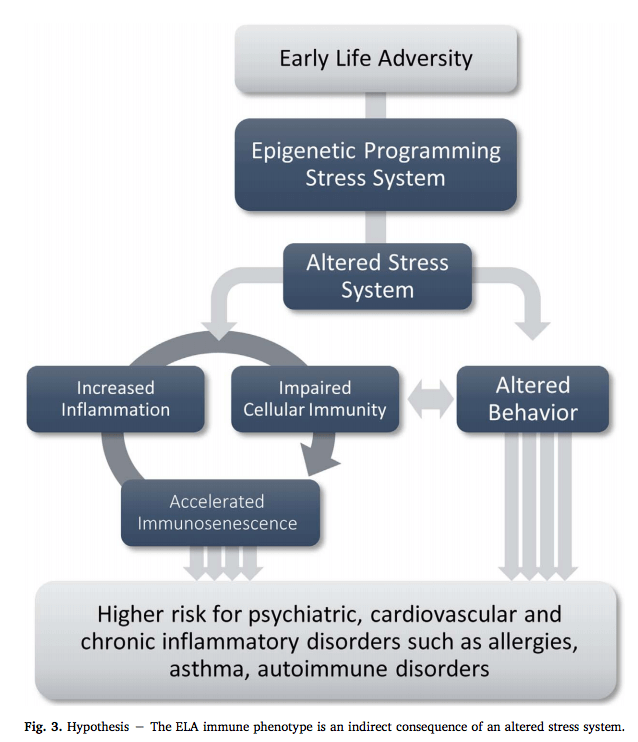
There is hope: Anyone can heal from childhood trauma
Roughly 65 percent of adults have an ACE score of at least one. Most individuals who have experienced childhood trauma have an awareness of this trauma, but may tend to downplay the extent and severity of their experiences. For this reason, taking the ACE quiz can help get a better grasp of one’s adverse experiences. It may also increase one’s understanding of the need for treatment and prevention of poor health outcomes.
Three out of four of the experts we communicated with for this article said that EMDR (Eye Movement Desensitization and Reprocessing) is an excellent form of treatment for those with a history of childhood trauma. Vincent Felitti, lead researcher of the ACE Study, also listed EMDR as his top suggestion for those seeking to heal from adverse childhood experiences.
Another recommendation we received was yoga and meditation. “Treatment starts with learning how to regulate the body,” Christine Fuchs, a licensed mental health counselor in New York, told us. This “can include things like yoga and deep breathing.” According to Fuchs, these forms of treatment aid in self-regulation and the ability to relax the body. This adequately sets the stage for addressing traumatic memories. Relaxing the body can also have profoundly beneficial effects on the stress response system over time.
Nancy Brooks of Nancy Brooks Counseling in Lancaster, Pennsylvania told GLP that “treatment of any disorder is best when it addresses the individual’s needs, which always includes understanding their current symptoms, what they have tried in the past, and what has and has not worked.” Since experiences of early adversity are not always accessible to memory, it’s important to remember that treatment can take place even in those who do not recall details of their trauma. Symptoms like anxiety can be treated with medication or Cognitive Behavioral Therapy, Brooks said.
Allison Johanson, a licensed clinical social worker from Supported Change LLC in Centennial, Colorado, added that since a need for control can often cause anxiety, depression, and behavioral difficulties in those with high ACE scores, “acceptance treatments such as Acceptance Commitment Therapy and Dialectical Behavioral Therapy have been proven to be effective.”
For those who wish to try EMDR but have limited time or financial constraints , virtual EMDR may be a cost-effective alternative.
Kristen Hovet is a journalist and writer who specializes in psychology, health, science and the intersection of sociology and culture. Follow her on her website, Facebook or Twitter @kristenhovet
This article originally appeared on the GLP on November 14, 2017.































