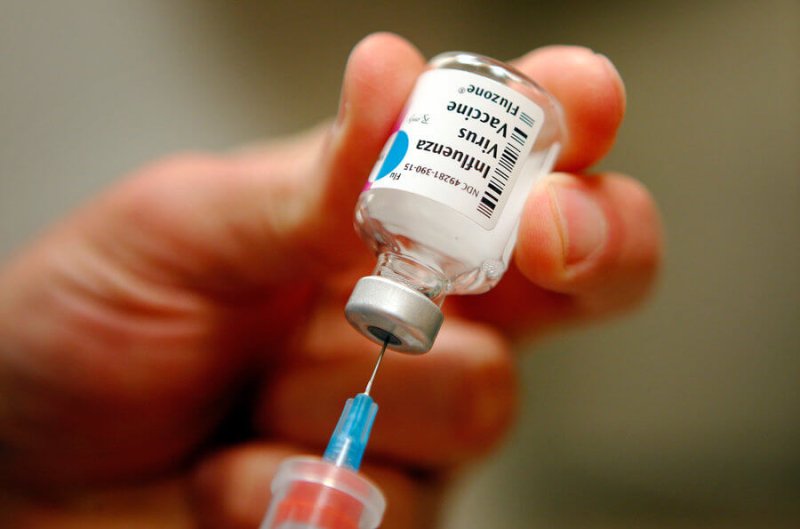
Given how genes have a hand in practically every health issue, it should be no surprise that studies are starting to show that not all people are the same in terms of how well a vaccine works. But a recent study examining responses to influenza vaccine does more than just tell us how to know who should feel more at ease after getting their seasonal flu shot. It actually suggests a tactic for intervening at the genetic level in those who are not good vaccine responders. At the same time, it lays the groundwork for personalizing preventive treatment, not just of flu, but also a host of other conditions.
In the years to come, it is likely that we’ll want to reexamine our immunization policies to account for variations in the effectiveness of different vaccines throughout the population. In addition to continuing a strong emphasis on the need to get vaccinated, the new approach will likely add tests for vaccine-relevant genes, and drugs to help the vaccines work better in certain people.
“Normal” gene works against flu vaccine
A study conducted recently at the University of Basel in Switzerland adds to findings from a series of other trials over the years looking at a gene called IL28B. In it’s most common form–what’s called “normal” in genetics–the IL28B makes a protein that inhibits immune cells called T-lymphocytes and B-lymphocytes from producing something called IL-4. But we carry two copies of every gene, and people in whom at least one of the IL28B copies is modified respond better to flu vaccine compared with those carrying two normal IL28B genes. Responding better means that their immune system learns to recognize flu virus, so is able to fight it off and keep the individual from getting sick.
It turns out that people with poor health status, such as those who are immunocompromised, tend possess two normal copies of the IL28B gene. This group of people also does not respond well to flu vaccine –a cruel irony since they are the people who need flu protection the most. In contrast, the Basel study found that healthier people tend to have one or two copies of the modified IL28B gene, and that these people’s immune systems respond very well to flu vaccination. That’s because the modified IL28B gene makes a defective protein that does not block the production of IL-4 in T- and B- lymphocytes.
Intervening at the genetic level
While it may sound frustrating that the very patients most in danger from flu are genetically prone to poor vaccine response, the Basel study also found that drug therapy is possible to make the poor vaccine responders into good responders. To prevent T- and B-lymphocytes from making the needed Il-4, the protein made by the IL28B gene protein must bind a certain receptor on the lymphocytes. The team found that simply giving a drug that blocks the IL28B receptor prevents the inhibition, thereby allowing the IL-4 production to proceed as it would in healthy individuals.
Mainstream media are generally good in explaining to the public that the medical and scientific communities are united in recommending a range of vaccines broadly to promote public heath, and that controversy to vaccine use comes only from fringe elements. Even so, the issues can still be confusing. Overall, the benefits of getting immunized for any of a range of diseases far outweigh any risks of vaccine complications.
But highly publicized discussions surrounding possible reductions in effectiveness of particular vaccines can make the public skeptical overall of immunization strategies. Prime examples in recent history involve pertussis vaccine last year and flu vaccines for the current season. Vaccine effectiveness is bound to fluctuate–that’s the nature of vaccines, because of how they work. But, whenever there is a report of even slightly reduced effectiveness, anti-vaxers don’t lose the opportunity to spin it as a shocking scandal to promote their anti-vaccination agenda. All of this can generate a confusing environment for the lay person whose prime motive is merely to do what’s best for his or her own family. Rather than allowing this latest discovery to be twisted similarly, an appropriately nuanced explanation must be delivered to the public. Such a discussion must highlight the point that the growing understanding of the genetic factors stands to make vaccinations work even better than they already do.
Expansion to other diseases
Studies over the last few years have generated genetic findings relevant to vaccines against a host of infections other than influenza. Covering measles, mumps, rubella (MMR), hepatitis B, anthrax and even smallpox (which has been eradicated), the emerging field of personalized vaccines already has a name: vaccinomics–playing on word genomics in the same way that personalized drug treatment (pharmacogenomics) and nutrition (nutrigenomics) are doing. Not only do genomics-based approaches apply to development of vaccines to prevent various conditions; they also will be used increasingly in the field of therapeutic vaccines –more powerful immune system boosters given to those who are already sick. Thus, while current immunization guidelines are organized in terms of vaccine schedules built around age groups and risk factors, guidelines of the near future will likely include an additional dimension: your genes.
David Warmflash is an astrobiologist, physician, and science writer. Follow @CosmicEvolution to read what he is saying on Twitter.