Now, scientists are turning to a uniquely human advantage, the ability to think and reason, to solve the issue. Now, we’re tricking pathogenic microbes into killing themselves.
In April, a team of French scientists published a new kind of molecular trickery that selectively kills harmful and antibiotic-resistant bacteria without traditional antibiotics. The research, led by genomicist Rocío López-Igual and colleagues at the Pasteur Institute capitalized on mechanisms of gene regulation to trick Vibrio cholerae into producing self-destructive toxins. This approach could be adapted to target other microbes and reduce the need for antibiotics.

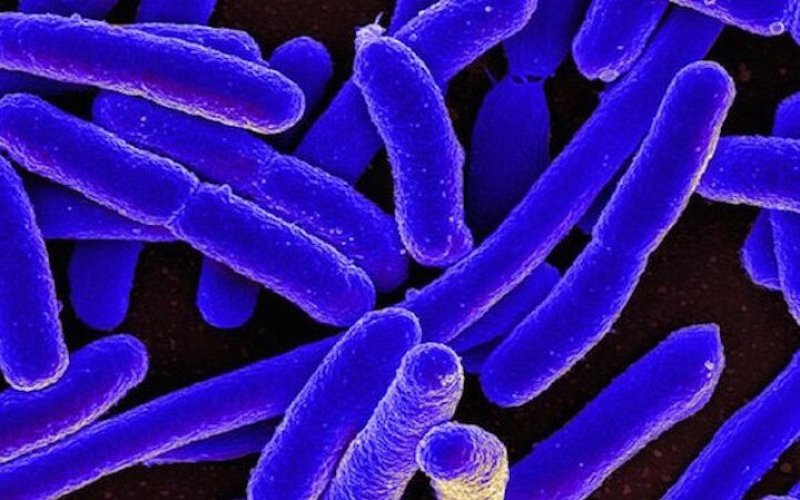
V. cholerae, which causes cholera, encodes multiple toxins in its genome. Bacterial toxins inhibit vital processes like DNA replication or cell division. Typically, anti-toxins – that the bacteria also produce themselves – protect bacteria from poisoning themselves. Stress activates the toxins, often leading to cell death. Although exactly why bacteria maintain deadly toxin genes is still puzzling, we know that artificially activating the toxins provides a route to kill bacteria. The star of López-Igual and her colleagues’ method is a toxin that inhibits DNA gyrase, an important bacterial enzyme. Normally, DNA gyrase relieves stress from twisted DNA strands, so preventing DNA gyrase activity causes breaks in DNA. And like in human cells, such severe DNA damage is also fatal to bacterial cells.
The researchers manipulated the DNA sequences of V. cholerae to create a code for production of the toxin in specific kinds of bacteria. The specificity of bacterial gene regulation ensures that only certain bacteria can interpret this code. Bad news for the ones that can: they end up triggering their own death.
In the new antimicrobial system, the expression of the toxin is controlled by a protein that also activates expression of V. cholerae’s virulence genes. Virulence describes a pathogen’s ability to make you sick. And since the virulence protein is present only in virulent bacteria, the antimicrobial will only harm virulent bacteria. So, the more dangerous the bacteria, the more likely it is to fall prey to its own toxin.
Scientists say that initiating what can be thought of as bacterial suicide by modifying their DNA might be the next workable solution to antibiotic resistance. In fact, a similar mechanism for killing the tuberculosis bacteria is currently being explored.
DNA-based antimicrobials like the one developed by Lopez-Igual and her colleagues avoid using antibiotic drugs that might only work temporarily. Because of the specificity of the antimicrobial, bacteria face less pressure to escape death and would need to change drastically in order to survive this self-destruct mechanism. While resistance to the antimicrobial could still arise, such resistance is much less likely than resistance to traditional antibiotics.
Additionally, this DNA-based method provides a platform for targeting other pathogens, like Staphylococcus aureus (which causes skin infections) and Streptococcus pneumoniae (pneumonia). The toxin from this paper targets V. cholerae using DNA sequences from V. cholerae’s own genome. Building from this model, scientists could manipulate the sequences from other bacterial genomes with similar results.
Finally, targeting specific bacteria also protects the natural microbiome. Traditional antibiotics used to treat infections kill everything in their paths, beneficial and harmful bacteria alike. Consequently, they impair common bacterial processes that keep our bodies working smoothly, like the digestion of fiber. Since depletion of the microbiome can be just as devastating as an infection, maintaining a healthy microbiome during the treatment of infections could improve recovery.
The team of French scientists warn that several obstacles must be overcome before employing this type of targeted-antimicrobial to treat human infections. First, they need an effective method to deliver the antimicrobial DNA to bacteria throughout the human body. Scientists also need to address the stability of the antimicrobial DNA, since mutations in the toxin could prevent it from functioning properly. Lastly, like current drugs, targeted antimicrobials will need to be assessed for safety. However, it is unlikely that human cells would be at risk.
Overcoming these barriers to the application of targeted-antimicrobials will provide us with a new weapon in the fight against antibiotic-resistant bacteria. As pathogens devastate human health, it might be time to turn the tables on them with a little deception.
Molly Sargen researches bacteriology at Harvard University.
A version of this article was originally published on Massive’s website as “Scientists have engineered a self-destruct button in bacteria“ and has been republished here with permission.