Mendel’s laws, like any laws in science, are wonderful because they make predictions possible. A woman and man both carry a recessive mutation in the same gene, and each of their children has a 25% chance of inheriting both mutations and the associated health condition. Bio 101.
In contrast to our bizarre new world of “alternate facts,” “multiple interpretations,” and “both are true” scenarios, science is both logical and rational. If an observation seems to counter dogma, then we investigate and get to the truth. That’s what happened for Millie and Hannah, whose stories illustrate two ways that genetic disease can seem to veer from the predictions of Mendel’s first law: that genes segregate, one copy from each parent into sperm and ova, and reunite at fertilization. (I’ll get to embryo engineering at the end.)
Millie’s situation is increasingly common – exome or genome sequencing of a child-parent “trio” reveals a new (“de novo”), dominant mutation in the child, causing a disease that is genetic but not inherited.
Hannah’s situation is much rarer: inheriting a double dose of a mutation from one parent and no copies of the gene from the other.
Millie and Bainbridge-Ropers syndrome
Millie McWilliams was born on September 2, 2005. At first she seemed healthy, lifting her head and rolling over when most babies do. “But around 6 months, her head became shaky, like an infant’s. Then she stopped saying ‘dada’,” recalled her mother Angela.
By Millie’s first birthday, her head shaking had become a strange, constant swaying. She couldn’t crawl nor sit, had bouts of irritability and vomiting, and bit her hands and fingers.
In genetic diseases, odd habits and certain facial features can be clues, but none of the many tests, scans, and biopsies that Millie underwent lead to a diagnosis. Nor were her parents carriers of any known conditions that might explain her symptoms. Still, it was possible that Millie had an “atypical presentation” of a recessive condition so rare that it isn’t included in test panels.
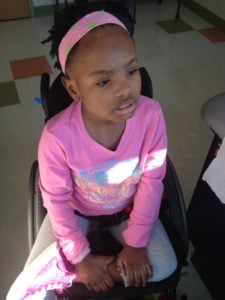
By age 6 Millie couldn’t speak, was intellectually disabled, and was confined to a wheelchair, able to crawl only a few feet. Today she requires intensive home-based therapies. But Millie can communicate. “She likes to look at what she wants, with an intense stare,” said Angela. She loves country music and Beyoncé, and every once in awhile something funny will happen and she’ll break into a big smile.
Millie’s pediatrician, Dr. Sarah Soden, suggested that trio genome sequencing, just beginning to be done at Children’s Mercy Kansas City (where the child already received care) as part of a long-term project, might help to assemble the clinical puzzle pieces to explain the worsening symptoms. So the little girl and her parents, Angela and Earl, had their genomes sequenced in December 2011. Analyzing the data took months, but Dr. Soden’s team finally found a candidate mutation in the child but not her parents. However the gene, ASXL3, hadn’t been linked to a childhood disease. Yet.
It’s typically a matter of time for gene annotation to catch up to sequencing efforts and clinical clues. In February of 2013, a report in Genome Medicine described four children with mutations in ASXL3 who had symptoms like Millie’s. Even her facial structures – arched eyebrows, flared nostrils, and a high forehead – matched those of the other children, as well as the hand-biting. They all have Bainbridge-Ropers syndrome.
One copy of Millie’s ASXL3 gene is missing two DNA bases, creating an inappropriate “stop” codon and shortening the encoded proteins. From this new glitch somehow arose the strange symptoms. Because neither Earl nor Angela has the mutation, it must have originated in either a sperm or an egg that went on to become Millie.
Since the paper about Bainbridge-Ropers syndrome was published three years ago, a few dozen individuals have been diagnosed and families have formed a support group and a Facebook page. That’s huge. Even if a disease has no treatment, as is the case for Bainbridge-Ropers, families find comfort in reaching the end of the diagnostic odyssey and locating others. Said Angela, “It was a relief to finally put a name on it and figure out what was actually going on with her, and then to understand that other families have this too. I’ve been able to read about her diagnosis and what other kids are going through.”
Hannah and GAN
Hannah Sames will be celebrating her 13th birthday next month, and is showing what may be early signs of strength in her muscles after receiving gene therapy into her spinal cord last summer to treat giant axonal neuropathy (GAN).
When I first met Hannah’s mom Lori in 2010, she told me that Hannah had inherited the exact same deletion mutation in the gigaxonin gene from her and her husband Matt. At that time, only a few dozen children were known to have the condition, and that number hasn’t risen much. Because of the disease’s rarity, I politely asked if Lori and Matt could be cousins but not know it. Shared ancestry seemed a more likely explanation for two identical extremely rare gene variants occurring in the same child than the parents having the same length deletion just by chance. But no, Matt and Lori aren’t related.
The answer came just a few months ago: Hannah inherited both of her gigaxonin deletion mutations from Lori, and none from Matt. This is a very rare phenomenon called uniparental disomy (UPD), meaning “two bodies from one parent.” Like Millie, UPD seemingly defies Mendel’s law of segregation, with a pair of chromosomes (or their parts) coming solely from one parent, rather than one from each parent.

UPD happens during meiosis, the cell division that sculpts egg and sperm. And it requires two exceedingly rare events: Two of Lori’s chromosome 16s ended up in an egg in which Matt’s chromosome 16 was lost. Hannah essentially inherited her mom’s mutation twice, without the protection of her father’s normal chromosome 16. This is especially likely with this particular chromosome because an extra copy of #16 —trisomy 16 — is the most common extra-chromosome condition associated with miscarriage.
Neither Millie’s Bainbridge-Ropers syndrome nor Hannah’s GAN actually counters Mendel’s law. Although Millie didn’t inherit her mutation, if she were able to have children, she would pass it on with a probability of 1 in 2 to each child, just like the law predicts for dominant inheritance. Likewise, a child of Hannah would inherit one copy of the mutation that causes GAN when present in a double dose, just like the law predicts for recessive inheritance.
Forget editing the germline genome and help sick kids
As I was writing this post, the National Academy of Sciences released its long-awaited tome on what’s being called, among other things, “embryonic engineering.” Rather than banning editing of the human germline forever, the report foresees certain situations in which gene or genome editing, using CRISPR-Cas9 or some other variation on the theme, might be deployed to prevent disease.
 While I think it’s great that the rare scenarios in which genome editing might be useful are finally being spelled out, instead of flaming fears of genetic enhancement spawning designer babies, my thinking about Millie and Hannah made me wonder why we would ever need to edit a genome to prevent disease in the first place. To quote the eminent mathematician from Jurassic Park, Ian Malcolm, “Yeah, yeah, but your scientists were so preoccupied with whether or not they could that they didn’t stop to think if they should.”
While I think it’s great that the rare scenarios in which genome editing might be useful are finally being spelled out, instead of flaming fears of genetic enhancement spawning designer babies, my thinking about Millie and Hannah made me wonder why we would ever need to edit a genome to prevent disease in the first place. To quote the eminent mathematician from Jurassic Park, Ian Malcolm, “Yeah, yeah, but your scientists were so preoccupied with whether or not they could that they didn’t stop to think if they should.”
Preventing illness in a future child of course isn’t the same as designing theme park dinosaurs, but like Jurassic Park’s technology, I can’t imagine why genome editing at very early developmental stages is necessary. Even for an exceedingly rare family situation in which passing on an inherited disease is unavoidable, according to Mendel’s laws, there are alternatives, although they do not yield a “biological” child: replace, select, or adopt:
An assisted reproductive technology can replace the sperm (intrauterine insemination) or egg (egg donation or surrogate using her own eggs) of the mutation carrier.
- Preimplantation genetic diagnosis can select embryos conceived in vitro free of either an inherited or spontaneous mutation. So we already have quality control of embryos.
- Adoption is an obvious alternative to designing a child.
Instead of replacing errant genes early in prenatal development, or even before, I think we should focus on helping the Millies and Hannahs who are no longer fertilized ova or early embryos, but are kids. That’s already starting for Hannah, thanks to the gene therapy technology that has been gestating since 1990. Millie’s turn hasn’t come yet.
So yes, let’s set rules for editing the human germline – but also consider whether this type of intervention will ever make sense in our overcrowded world.
This article originally appeared on the PLOS DNA Science blog under the title Defying Mendelian Genetics and “Embryo Engineering” and has been republished with permission from the author.
Ricki Lewis is a long-time science writer with a PhD in genetics. She writes the DNA Science blog at PLOS and contributes regularly to Rare Disease Report and Medscape Medical News. Ricki is the author of the textbook Human Genetics: Concepts and Applications (McGraw-Hill, 12th edition out late summer); The Forever Fix: Gene Therapy and the Boy Who Saved It (St. Martin’s Press, 2013) and the just-published second edition of Human Genetics: The Basics (Routledge Press, 2017). She teaches Genethics online for the Alden March Bioethics Institute at Albany Medical College and is a genetic counselor at CareNet Medical Group in Schenectady, NY. You can find her at her website or on Twitter at @rickilewis































