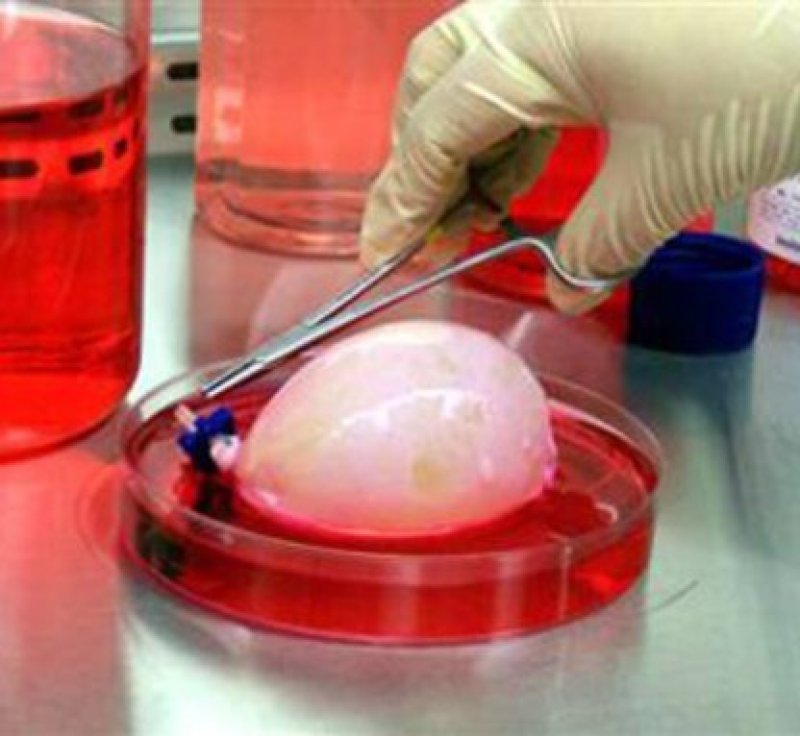
The concept behind tissue engineering is simple: grow the patient’s stem cells in the laboratory, add them to a scaffold material, and you have a laboratory-grown organ. But few patients have benefited from this technology so far. Could change be on the horizon?
…
To address [various complications], a research team from the Wake Forest Institute for Regenerative Medicine in Winston Salem, NC, has been developing new therapies for both anal sphincter injuries and short bowel syndrome.
But what is the likelihood of these new therapies ever reaching the patients, many of whom are in desperate need of better treatment options?
…
Dr. Bitar’s, Khalil N. Bitar, Ph.D., a professor of regenerative medicine team has spent years developing a precise method that allows [him and his team] to grow muscle cells that are precisely aligned in one direction, and connect with nerve cells when they are added to the cell culture a few days later.
…
Their latest study…demonstrates the feasibility of using an engineered anal sphincter in a large animal model to restore fecal continence…
In fact, most areas of tissue engineering suffer from the problem of scaling. Even though therapies may work very well on the scale of small rodents, making much larger constructs – such as stretches of small intestine for humans – is much more challenging.
The GLP aggregated and excerpted this blog/article to reflect the diversity of news, opinion, and analysis. Read full, original post: Are engineered organs finally becoming reality in medicine?