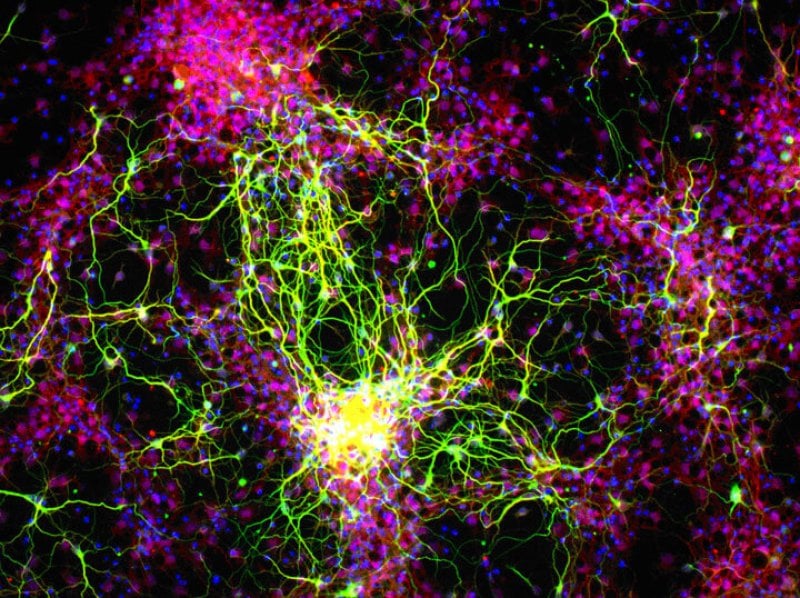
A 7-year-old boy whose outer skin layer was nearly gone due to a genetic disease has had it replaced, using his own genetically-modified stem cells, report researchers from Germany, Austria, and Italy in Nature.
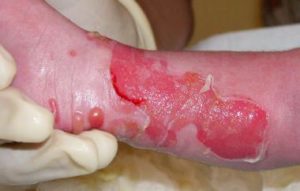
He has junctional epidermolysis bullosa (JEB). The thin tissue layer separating the epidermis from the dermis below is extremely fragile, causing blistering, peeling, and fraying of the skin, leaving wounds that can be deadly and raising the risk of skin cancer. The researchers replaced the boy’s shattered skin with grafts to his limbs and then the back of his body, followed by closing some of the gaps. In essence, they engineered and knit him a new epidermis – with a lot of help from the boy’s own capacity to heal.
Skin layers separate
JEB arises from mutations in any of several genes that encode proteins that hold the epidermis to the dermis. The boy’s mutation is in the gene LAMB3, one of three that instruct epidermis cells to make laminin-332, a protein that links the layers. About 40 percent of patients with JEB don’t reach their teens. In the US, fewer than one in a million people has JEB.
Healthy epidermis turns over every month, thanks to stem cells. In 2006, Michele De Luca, MD, from the Center for Regenerative Medicine at the University of Modena and Reggio Emilia in Italy and colleagues reported in Nature Medicine on introducing working copies of LAMB3 aboard retroviruses into skin stem cells sampled from a man with JEB, fashioning grafts patched onto nine small areas of his legs. The grafts took within eight days, and a second patient did well too. But the fix wasn’t extensive enough to make life noticeably easier.
The new work takes a giant step forward, to “demonstrate life-saving regeneration of virtually the entire epidermis” of the boy, according to the report. The researchers again used retroviruses to introduce healthy LAMB3 genes into stem cells sampled from the limited parts of the boy’s epidermis still clinging to the layers below. Three of the researchers discussed their work in a press conference yesterday.
The procedure
The boy was admitted to the burn unit of Children’s Hospital at Ruhr University in Bochum, Germany, in June 2015. He’d had the blisters of JEB since birth, but they’d gotten much worse from bacterial infections. Soon after he arrived, about 60 percent of his epidermis fell off.
“The first few days we just tried to keep him alive,” recalled Tobias Hirsch, MD, from the burn center. That meant meticulously changing dressings, giving antibiotics, tube feeding, and trying synthetic skin and grafts of the father’s skin. Nothing helped. “After two months we thought he would die, so we changed to palliative care. But his parents asked us to try anything.” That’s when they sought the genetically modified stem cell grafts that De Luca’s team was pioneering, telling the parents that the boy might not survive.
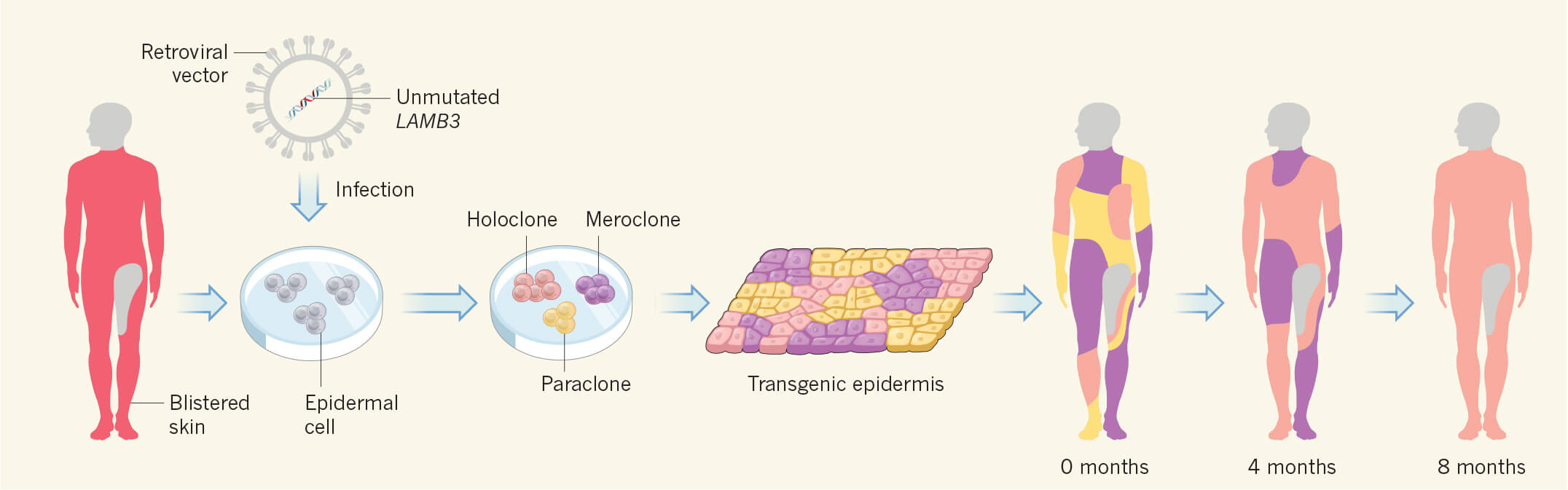
They began with a 1½-inch square patch of healthy-looking skin from the boy’s groin area, grew cell cultures, then added the retroviruses bearing the working copies of the gene. Three types of patches formed. Those harboring stem cells are called holoclones, those with specialized cells are paraclones, and patches with partly specialized cells are termed meroclones. Nevertheless, only the holoclones persisted.
“We transferred the grafts beginning in October 2015. Within five weeks, the cells had covered about 80 percent of the boy’s body,” explained De Luca. Individual grafts, one-cell-thick and 1.2 to 3.2 square feet in area, were gently applied to prepared “wound beds,” where the natural bacterial residents had been removed and thread-like fibrin protein laid down, which prevents shrinkage before dissolving. No stitching or sticking required.
Like paint spreading over a canvas, the “epidermal islands” covered most of the boy’s body. After the limbs and back, the doctors filled in recalcitrant areas on the thighs, throat, right hand, and shoulders in a third procedure. And the new skin held up to touch that would formerly have triggered blistering.
Success
The doctors expected the worst, but the grafts quickly took and the boy was well enough to leave the hospital in February 2016, returning quickly to a near-normal life of school and sports. Then the stem cells in his new epidermis spawned hairs and sweat glands, as such cells normally would. This isn’t the case for a full-thickness burn, which destroys much more of the skin. And the boy didn’t need to apply ointment daily as burn patients must.
Two years after the procedure, some 20 cell divisions later, “all biological and clinical measures were fine, stable, robust, and the skin functionality is quite good,” De Luca said. Only some stem cells remain, apparently enough to keep the skin going. The boy’s immune system hasn’t rejected the cells, which are genetically identical to the rest of him, nor did the normal genes insert in ways that could cause cancer.
“His skin is smooth. Bruises heal as in a normal kid, in 12 to 14 days. He still has some blisters in non-transplanted areas, in about 2 to 3 percent of his body where we didn’t transplant,” said Tobias Rothoeft, MD, also of University Children’s Hospital. Only a few bits of skin, on his left armpit, upper shoulders, buttocks, and right thigh, remain fragile.
Biopsies taken at four,eight, and 21 months after the procedure continued to show the doctored stem cells doing their jobs, although “we can’t take too many biopsies because he’s a patient, not a mouse,” De Luca said.
The treatment might be deemed too extreme for many patients and was done on this patient to save his life, but introduced in stages could make life much easier for people with this form of JEB, the researchers write. They envision banks of GM stem cells begun at birth, providing a ready store of replacement skin.
The now 9-year-old’s customized stem cells are indeed stored in the lab, ready in case he needs a patch someday. “That’s a fantastic option for me as a surgeon because I can get as many stem cells as needed to cover all open areas,” Hirsch said.
The family would probably agree that the results are indeed fantastic.
Ricki Lewis has a PhD in genetics and is a genetics counselor, science writer and author of Human Genetics: The Basics. Follow her at her website or Twitter @rickilewis.