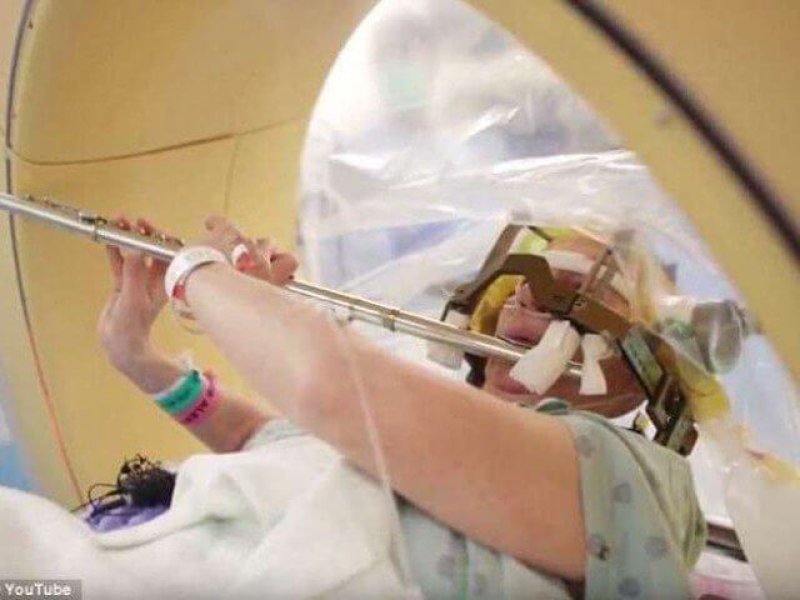
In this instance, Anna Henry is a professional musician who has endured tremors since childhood. With recent worsening now impacting her passion and life’s work, she took the leap and was operated on at Memorial Hermann-Texas Medical Center in Houston. (See video here).
Albert Fenoy, M.D., neurosurgeon with the Mischer Neuroscience Institute at Memorial Hermann-Texas Medical Center and UTHealth, who specializes in the procedure maintains,
“Deep brain stimulation is a really fantastic tool in how we can modulate a perturbed, dysfunctional system in the brain and make it more normal.”
What is Deep Brain Stimulation?
DBS is quite an amazing option for eligible candidates with certain movement disorders and neuropsychiatric conditions, including but not limited to Parkinson’s Disease, Essential Tremor, Epilepsy and more recently Obsessive-Compulsive Disorder. Research is underway for the potential uses in other diseases. That said, it is not a simple procedure or without risk (e.g. infection, bleeding, stroke, seizures) since it occurs in a premier real estate location.
Typically reserved for those whose conditions are refractory to medication, it is an invasive intervention. An opening is made by drilling into the skull to allow tiny electrodes to be inserted deeper within the brain. First, detailed brain mapping is performed with imaging studies and monitoring equipment to identify the main locus causing the problem. Those whose issues arise from a more isolated spot are more likely to succeed with this surgery than those who might have multiple areas of origin. Next steps involve shaving the head and securing an external contraption usually referred to as a halo which gets literally screwed into the scalp.Think of this apparatus like the mechanism that surrounds a globe and serves to measure longitudes and latitudes to guide surgeons with proper placement of their electrodes. In other words, it permits targeted neuro-navigation.This stereotactic head frame also keeps your head still during the surgery.
Multidisciplinary teams assist the neurosurgeon in these cases. Neurophysiologists and neurologists enter the surgery when the electrodes have been inserted so they might test varying levels of current or stimulation necessary to stop the tremor in that particular patient. The patient does not feel pain as she is monitored and medicated by anesthesiologists. But, she must remain awake since this interactive state is critical to fixing the underlying issue and avoiding complications.
Determining the amount of necessary sustained voltage for the particular patient’s issue and guaranteeing vital structures are not impeded upon requires incremental changes that are safely performed. Having the patient speak or perform tasks like bringing a cup of water to the mouth – or in this case playing the flute, are markers for preserving a person’s speech center or curtailing side effects while testing the extent of tremor cessation.
Once the ideal parameters are set to regulate abnormal electrical activity, for example, and the surgery proves effective, the electrodes are secured and threaded under the skin to an implanted pacemaker type device in your chest that can be adjusted when need be as an outpatient.
Is it a cure?
DBS does not cure the disease, but rather the symptom that is adversely impacting you. Sometimes it is enough to suppress the problem, other times it is used in combination with medications. It requires continued monitoring and alterations in the degree of stimulation. People can have sides effects of balance issues or confusion, for instance, so are followed regularly.
In conclusion
The first residency I started was neurosurgery. As a medical student, I did research in deep brain stimulation. Though this was many years ago at this point, it is no surprise that such a case of a flute-playing patient under these circumstances is so compelling. It was then and continues to be as it represents some of the most substantial strides we have made in medical progress. Back then, the cases were incredibly long and the process very tedious as one could imagine. But, each and every time you reached the pivotal moment in surgery and witnessed a person you had seen disabled and impaired by their tremor instantly steady their hand, it took your breath away. You knew their life had forever changed and for the better.
It is comforting to know these types of marvels in innovation and dedication still do take our collective breath away.
Dr. Jamie Wells, MD, FAAP, is a Board-Certified physician with over a decade of experience caring for patients and the Director of Medicine at the American Council on Science and Health. She served as a Clinical Instructor/Attending at NYU Langone, Mt. Sinai-Beth Israel and St. Vincent’s Medical Centers in Manhattan. Follow her on Twitter @jamiewellsmd.
A version of this article was originally published on the American Council on Science and Health’s website as “Woman Plays Flute While Undergoing Brain Surgery, Video Goes Viral” and has been republished here with permission.