About 5.4 million tests have been done in the US, according to the COVID Tracking Project, in a population of 328.2 million. That might sound like enough to keep ahead of an infectious disease that has “only” killed in five figures, but such an assumption grossly oversimplifies the situation.
Controlling the pandemic in the US is going to require a daunting number of diagnostic tests – not just for the sick, but to verify when they’re better (two tests 24 hours apart for hospital discharge), in contact tracing to limit spread, and in the many individuals who’ve been infected but have few or no symptoms.
“In a few countries, the use of diagnostic testing on a massive scale has been a cornerstone of successful containment strategies,” write Matthew P. Cheng, MDCM. McGill University Health Centre and colleagues in a recent article in Annals of Internal Medicine. The US isn’t on that list and has been struggling to catch up.
Simply put, we need faster, cheaper and more accurate tests than what we currently have. If they can be administered at home or in informal settings, all the better. Among the potential solutions for this challenge are efforts to turn everyone’s favorite gene editing tool, CRISPR, against the coronavirus. If successful, we could see a shift in access to tests. Imagine being able to use a nasal swab that delivers a “yes” or “no” verdict on coronavirus infection in under 40 minutes — essentially like a home pregnancy test.
A CRISPR-based diagnostic is in the sights of researchers at the University of California, San Francisco Medical School and Mammoth Biosciences, which recently revealed plans for an inexpensive, compact test.
“I can run it now myself at home,” said Dr. Charles Chiu, professor of laboratory medicine at UCSF and co-lead developer of the new test, in an interview with NPR. Still, he acknowledged the test, which is being submitted for FDA approval, isn’t yet simple enough for the average person to operate. He expressed confidence that a home-based test for nonexperts is within reach.
“What we really want to develop is something like a handheld, pocket-sized device using disposable cartridges,” he told NPR.
So, where would such CRISPR-based tests fit within the universe of coronavirus diagnostics? There’s little reason to think they would replace other testing options. Rather, think of them as offering another option for hospitals, clinics, doctors, and even consumers. That said, let’s take a look at where we are in testing.
A testing timeline
Diagnostic tests use a version of the polymerase chain reaction (real-time reverse transcriptase PCR) to amplify pieces of the RNA genome of SARS-CoV-2, the virus behind COVID-19. Dr. Deborah Birx, Coronavirus Response Coordinator, suggested that antigen-based tests be added to increase the supply, but these detect protein antigens on the viral surface, not the genetic material, and may be less likely to indicate infectious virus. For influenza diagnostic testing antigen tests are less accurate than the PCR-based tests.
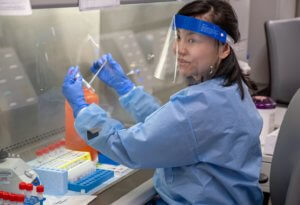 PCR is simple in concept, but not always easy to carry out. It requires raising and lowering the temperature repeatedly as nucleic acid sequences are copied. Reagents may run out, and it requires specialized equipment. A PCR-based test that could diagnose infection in a few hours often takes more than a day because the sample must be sent to a lab.
PCR is simple in concept, but not always easy to carry out. It requires raising and lowering the temperature repeatedly as nucleic acid sequences are copied. Reagents may run out, and it requires specialized equipment. A PCR-based test that could diagnose infection in a few hours often takes more than a day because the sample must be sent to a lab.
False negatives can occur if viral RNA in a sample degrades during shipping, or if not enough collects on the swab. If either happens and a patient worsens, another test is required. But if the virus descends into the lungs, not enough may remain in the throat for a test to pick it up, even though the patient is actually sicker.
And so some people with obvious symptoms of COVID-19 must have two or three tests before a result is positive.
But PCR-based tests are what we have. Regulations shifted into emergency mode to bolster supplies.
On February 4, the Food and Drug Administration (FDA) greenlighted the Emergency Use Authorization (EUA) of the Center for Disease Control and Prevention’s (CDC) PCR test, making it available to to state and local public health labs and the Department of Defense. The EUA enables rapid roll-out of a still-experimental test. Even though PCR has been used in clinical diagnostics for decades, the virus is new and therefore so is the test.
A PCR-based diagnostic for COVID-19 amplifies RNA sequences unique to the novel virus, as well as gene parts common to other coronaviruses and a control sequence (encoding an enzyme, RNase), to make sure the test is working.
But at the end of January, bits of viral RNA in the CDC facility tainted some of the first test kits, so that they could yield false positive results, delaying their use.
On February 28, FDA took further action, announcing that clinically-licensed labs can use in-house developed tests while awaiting the EUA. These labs are “CLIA-compliant,” which means that they satisfy the standards of the Clinical Laboratory Improvement Amendments set by the federal government.
So places like Meridian Health, the Cleveland Clinic, Stanford Medicine, and many others began to do part of the PCR work-up, so that they didn’t have to outsource samples. It was a little like people addicted to going to Starbucks learning how to make their own brew at home – maintaining standards but taking on more of the task. (In fact, a study was just published on how to make the healthiest at-home brew.)
Michelle N. Gong, MD, Chief of Critical Care Medicine at Montefiore Medical Center in the Bronx, said on a JAMA Network webinar on March 23 that bringing the testing in-house immediately escalated testing.
“We started with sending samples to the Department of Health, but it became increasingly clear that it was not going to be adequate. It took days. Our hospital’s epidemiologist worked to bring testing onsite and that has changed the game. The ability to test onsite and turn it around fast made it much more efficient to get patients what they need.”
The FDA’s list of diagnostics granted EUA status continues to grow. The last time I checked it had 62 entries.
On March 27, the EUA granted Abbott Labs use of a test that they had under development that detects two viral genes (N and RdRp), one of them different from the CDC’s recipe. According to the company, the test can deliver positive results in 5 minutes and negative results in 13 minutes.
The Abbott test runs on an existing platform, ID NOW, and uses a gene amplification technology that doesn’t require the temperature shifts of PCR. The test is done in a lightweight box about the size of a toaster that’s already used in doctors’ offices, urgent care facilities, and emergency departments to rapidly diagnose influenza, strep, and respiratory syncytial virus.
But the company’s initial forecast of providing 50,000 tests a day, starting soon, may need to await further validation. A researcher at the Cleveland Clinic, Gary Procop, MD, tested five products on 239 patient samples known to be positive for COVID-19. Abbott’s test missed 15 percent.
The World Health Organization (WHO) also provided many tests early on and continues to do so.
On April 21, FDA re-deployed the Emergency Use Authorization of LabCorp’s PCR-based test for use in a home-kit that the company provides. It’s being rolled out for health care workers first; consumer tests may follow in a few weeks.
Another way to boost test kit supplies is to harness the gene editing tool CRISPR. It may be faster and simpler than PCR.
A Mammoth effort
The team from Mammoth Biosciences and UCSF reported on “CRISPR–Cas12-based detection of SARS-CoV-2” in April 16’s Nature Biotechnology. Company co-founder is Jennifer Doudna, PhD, co-inventor of CRISPR.
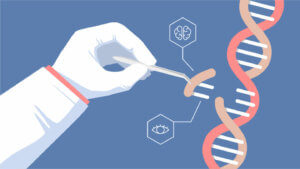 Mammoth’s “visual readout strip” works at the bedside, is fast, and in trials so far, picks up 100% of negatives and 95% of positives – although much more extensive evaluation is needed. The report considers findings in 36 patients with COVID-19 and 42 people with other respiratory illnesses.
Mammoth’s “visual readout strip” works at the bedside, is fast, and in trials so far, picks up 100% of negatives and 95% of positives – although much more extensive evaluation is needed. The report considers findings in 36 patients with COVID-19 and 42 people with other respiratory illnesses.
On February 15 Mammoth unveiled the protocol for their “point of care” test in a white paper that describes it as useful “in areas at greatest risk of transmitting SARS-CoV-2 infection, including airports, emergency departments, and local community hospitals, particularly in low-resource countries.”
“We need faster, more accessible and scalable diagnostics. The point-of-care testing space is ripe for disruption and CRISPR diagnostics have the potential to bring reliable testing to the most vulnerable environments,” said Mammoth’s Chief Technology Officer Janice Chen, PhD.
The test uses the company’s DETECTR technology; that stands for DNA Endonuclease-Targeted CRISPR Trans Reporter. The platform had already been in the works for human papillomavirus, described in a April 27, 2018 report in Science.
The company started revamping its system for the novel coronavirus as soon as cases were reported from Wuhan, and within two weeks was testing it on the first patient samples. “Because CRISPR can be programmed to detect any DNA or RNA sequence, we reconfigured our DETECTR platform within days to detect the SARS-CoV-2 virus from one of the first confirmed cases in the U.S.,” said Dr. Chen.
The system collapses the two steps of PCR-based tests into one: copying viral RNA into DNA and amplifying it fast, without temperature shifts. The test snips off a “reporter molecule” that generates the stain on the paper read-out strip, and uses the Cas12 enzyme, which makes more precise cuts than conventional Cas9.
 The test zeroes in on three gene pieces:
The test zeroes in on three gene pieces:
- Part of the nucleocapsid (N) gene that is in the CDC’’s test and is unique to SARS-CoV-2.
- Part of the envelope (E) gene that is the basis of the WHO’s test but is also seen in bat coronaviruses and the one that causes SARS.
- RNase P as a control – if it doesn’t show up, the test hasn’t worked.
It picks up 70 to 300 DNA pieces of genetic material per microliter of fluid from a nose or throat swab. A microliter is one-millionth of a liter.
Another CRISPR candidate: SHERLOCK
SHERLOCK™, for “Specific High Sensitivity Enzymatic Reporter Unlocking, is a testing platform coming from work on Zika virus disease and Dengue fever published in 2018 in Science. Sherlock Biosciences provides the test and Cepheid.com provides their GeneXpert® Systems cartridge device. The approach licenses work from the Broad Institute, home of another CRISPR founder, Feng Zhang, PhD.
 The system can identify any genetic target, and therefore any infectious disease. The test for COVID-19 may reach the market as a dip stick, paper strip, or even “an electrochemical readout that can be read with a mobile phone,” according to company information.
The system can identify any genetic target, and therefore any infectious disease. The test for COVID-19 may reach the market as a dip stick, paper strip, or even “an electrochemical readout that can be read with a mobile phone,” according to company information.
The system zeroes in on genome pieces unique to SARS-CoV-2 that encode the spike (S) protein and a “polyprotein” that commandeers the host cell. (My blog post from the start of the pandemic, “COVID-19 Vaccine Will Close in on the Spikes,” explains the genetic make-up of the virus.)
It uses powerful Cas12 and Cas13 enzymes and can reportedly detect down to the single molecule level. It’s fast, accurate, and works directly on body fluids. And with 23,000 GeneXpert Systems already at health care facilities, popping in a COVID test may be the best idea yet.
To biologists and many others it was clear from the start that fighting this pandemic would require far more testing than for just the people who show up at health care facilities with symptoms. An epidemic is a population phenomenon that must be addressed at that level. It is comforting to know that regulations were in place to allow implementation of variations on the testing theme, and that the companies that have long expected a viral pandemic are collaborating to rapidly adapt existing tests, tools and technologies to put the pandemic of 2020 behind us.
Ricki Lewis is the GLP’s senior contributing writer focusing on gene therapy and gene editing. She has a PhD in genetics and is a genetic counselor, science writer and author of The Forever Fix: Gene Therapy and the Boy Who Saved It, the only popular book about gene therapy. BIO. Follow her at her website or Twitter @rickilewis































