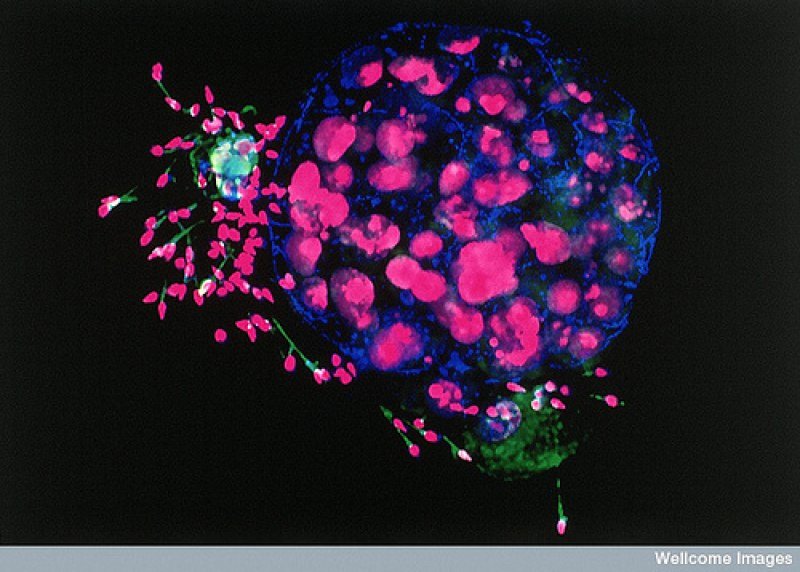
Genome editing of human fertilized eggs has revealed early embryonic events that differ in timing from those in mice.
“This is the first time that CRISPR-Cas9 genome editing has been used to study the function of a gene in human embryos, which can lead to improvements in stem cell biology, IVF treatment, and knowledge of how human embryos develop in the first window of seven days, perhaps revealing causes of when pregnancy fails,” said Kathy Niakan, a developmental biologist at the Francis Crick Institute in London and team leader, at a news conference yesterday. The work is reported today in Nature.
Basic research, not designer babies
The findings illustrate the potential power of CRISPR genome editing in basic research, in contrast to the report this summer on use of the technology by Shoukhrat Mitalipov, of Oregon Health & Science University, and co-workers to correct a mutation that causes a heart problem by targeting sperm as they enter eggs.
Instead, the new work continues the strategy of classical genetics to disrupt a gene to infer it’s normal function, but with better precision and efficiency. Applying CRISPR to explain basic biology and to treat disease starkly contrast with fears of its use for genetic enhancement or to “design” babies.
The researchers emphasize that they didn’t create embryos just to destroy them. “The donors of the embryos consenting for use in research see the benefit of this research. They want some good to come from these spare embryos, just as studies on human embryos led initially to develop IVF, from which they have benefited. They see that good comes from it,” Niakan said. And that’s facilitated in the UK, she added, because of “the clear and strict regulatory framework to work ethically on embryos to gain important insights that lead to advances in IVF.”
 When it comes to illuminating early human development, there’s nothing that measures up to using the real thing: human cells and tissues. Different species often use the same genes during early development, but according to different timetables. And timing is critical to assisted reproductive technologies like IVF, Niakan said.
When it comes to illuminating early human development, there’s nothing that measures up to using the real thing: human cells and tissues. Different species often use the same genes during early development, but according to different timetables. And timing is critical to assisted reproductive technologies like IVF, Niakan said.
Human and mouse embryos have similar overall shapes and the same key three first active genes. But there are also important differences, before as well as after implantation in the uterus. A mouse embryo implants at day four, and a human, seven to 10 days after fertilization.
Events that unspool even before a rapidly-dividing early embryo traverses the tube leading to the uterus are even more important. “Which key genes are absolutely essential for a human embryo to go from a fertilized egg to a blastocyst?” Niakan asked, referring to the hollow ball of cells that is a turning point in development. The team deployed CRISPR to harpoon the OCT4 gene in 41 human fertilized ova that had been deep-frozen five to 10 years ago as IVF “spares” donated for research.
OCT4 is one of a handful of genes whose encoded proteins guide the earliest steps of embryo formation. It’s one of the “Yamanaka factors used to sculpt induced pluripotent stem (iPS) cells from adult cells and is also essential for deriving human embryonic stem (hES) cells from early embryo cells.
Embryo forms
The experiments zeroed in on the first developmental “decision” – when cells become part of either the embryo or the supportive structures, such as the placenta and yolk sac. The fertilized ovum sequentially divides, yielding two, four, eight, and when it’s about 200 cells, forms a solid ball that then hollows out to become the blastocyst. Most IVF embryos don’t make it past this point, so it’s critical.
About day five after fertilization, a smear of a mere 20 cells nestles on the inner face of the blastocyst ball. These “epiblast progenitor cells” form the “inner cell mass” that goes on to fold and contort as the forming body elongates, limbs bud, and rudimentary organs form. The other cells become the placenta.
OCT4 protein appears by the 8-cell stage, and it’s known to be vital because of its importance in deriving iPS and hES cells. But researchers didn’t know exactly what it does, just that it acts earlier in human than mouse embryos.
Editing out OCT4: A developmental disaster
Sure enough, when CRISPR removed two DNA bases from human OCT4, the early embryos began a strange undulating movement, swelling and then collapsing like a cat regurgitating a hairball. Only 19 percent of the embryos survived past the blastocyst stage, compared to 50 percent for control embryos that received the microinjection without the CRISPR guiding parts.
 Sidelined OCT4 derails the exquisite timing of early development. Three key genes vital to establishing the distinctive layers of the embryo don’t work, while genes that are normally switched on later to sculpt specializations turn on too soon. It’s a mess.
Sidelined OCT4 derails the exquisite timing of early development. Three key genes vital to establishing the distinctive layers of the embryo don’t work, while genes that are normally switched on later to sculpt specializations turn on too soon. It’s a mess.
“The effect on the 20 epiblast progenitor cells, the precursor of the embryo, was different from mice. We would have never gained this insight had we not studied the function of this gene in human embryos. We also saw an effect on the precursor cells to the placenta that is completely different from the mouse,” Niakan said. Editing efficiency was about 80 percent.
A start
The results are a proof-of-principle that can be applied to interrogate other genes that are critical as an embryo gets ready to implant into its uterine home. And maybe learning what key genes do during that initial seven-day window, in humans, can increase the odds of IVF success from the current 12-13 percent of in vitro-fertilized eggs that develop beyond three months.
Despite the huge potential, the team says there’s more to explore with OCT4 before moving on to other genes. Said co-author James Turner, also from the Crick Institute:
We now know that OCT4 is important for formation of multiple lineages in the embryo. We’re interested in seeing how it’s regulating each of those lineages. For example, which genes induce formation of cells that give rise to the embryo proper versus the placenta?
Summed up Niakan: “This is the first genome editing used to study gene function in human embryos. It revealed the important role for OCT4 and we should study the roles of other genes to improve stem cell technology, IVF, and understanding the causes of pregnancy failure.”
Ricki Lewis has a PhD in genetics and is a genetics counselor, science writer and author of Human Genetics: The Basics. Follow her at her website or Twitter @rickilewis.