- Issue: Childhood vaccination rates fell worldwide during the COVID-19 pandemic. However, reductions in childhood vaccination were not universal, which may be related to differences in vaccine eligibility, vaccine hesitancy, and vaccine administration programs across countries.
- Goals: Explore how childhood vaccination rates changed during the COVID-19 pandemic in five high-income countries with varying approaches to vaccine policy.
- Methods: Surveys of in-country experts and analysis of secondary data sources in Australia, Germany, Singapore, the United Kingdom, and the United States.
- Key Findings and Conclusion: While vaccination rates fell worldwide during the COVID-19 pandemic, the high-income countries in our study maintained high childhood vaccination rates for polio and measles-mumps-rubella (MMR) near or above the herd immunity threshold (80% for polio and 95% for measles). Australia and Singapore, which have the strictest vaccine requirements, boasted the highest polio vaccination rates in both 2018 and 2021. No countries require the human papillomavirus (HPV) vaccination nationwide, but Australia, Singapore, and the U.K. have school-based HPV vaccination programs and high vaccination rates. Strong vaccine requirements, combined with school-based immunization or catch-up programs, may help boost childhood vaccination rates where they lagged during the pandemic.
Introduction
In 2022, public health authorities detected polio in wastewater in London and in New York, where a polio infection was also reported.1 Reductions in childhood vaccination rates during the COVID-19 pandemic and increasing vaccine hesitancy in the United States may have contributed to polio’s reemergence, as well as to measles outbreaks in the U.S. in 2024.2Across high-income countries, vaccine policies, including where routine vaccines are administered, vary significantly. The likelihood of parents or guardians delaying or refusing vaccines for their children also varies.3 These differences partly are a result of variation in the severity of the COVID-19 pandemic across countries and the extent of disruptions in preventive care, including childhood vaccinations.4 These factors may have contributed to the variability in vaccination rates during the pandemic across countries.
With support from the Commonwealth Fund and its network of international health care leaders,5 we explored differences in eligibility, administration, requirements, and pandemic-related disruptions for three routine childhood vaccinations: polio, measles-mumps-rubella (MMR), and human papillomavirus (HPV). We selected these vaccines because they are administered at different ages, face differing requirements and penalties, and were approved for use at different times.6 Our research focused on five high-income countries that have varying childhood vaccination policies: Australia, Germany, Singapore, the United Kingdom, and the United States. The selected countries are among those regularly studied by the Commonwealth Fund’s International Health Policy and Practice Innovations program.7
Key Findings
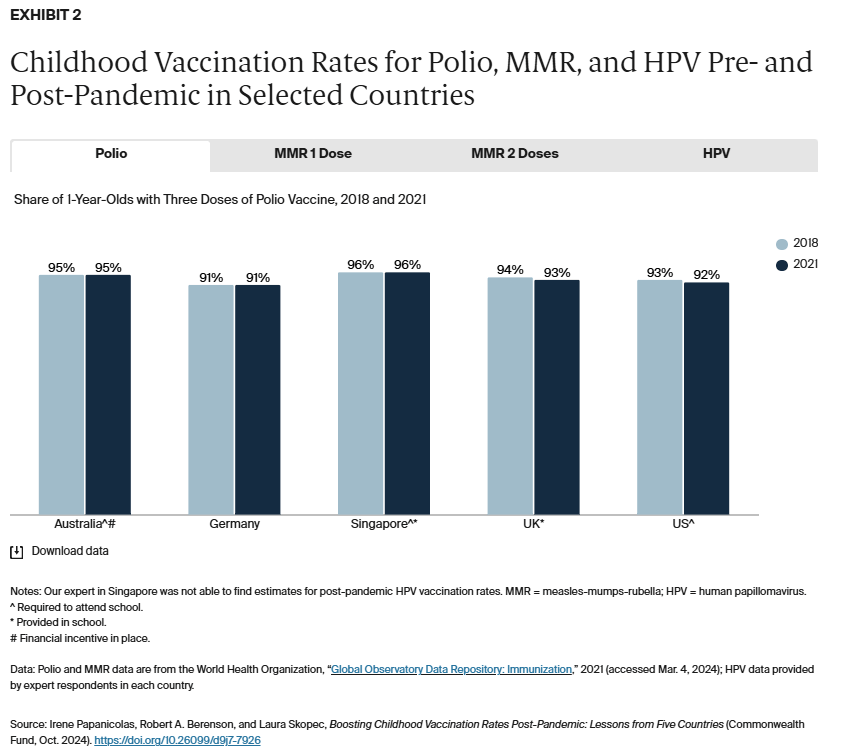
Childhood vaccination policies vary across the five countries and by vaccine type (Exhibit 1). Australia, Singapore, and the U.S. require polio and MMR to attend school, while Germany only requires MMR. Accordingly, Germany has higher immunization rates for MMR than polio, for which vaccination is not mandated (Exhibit 2).
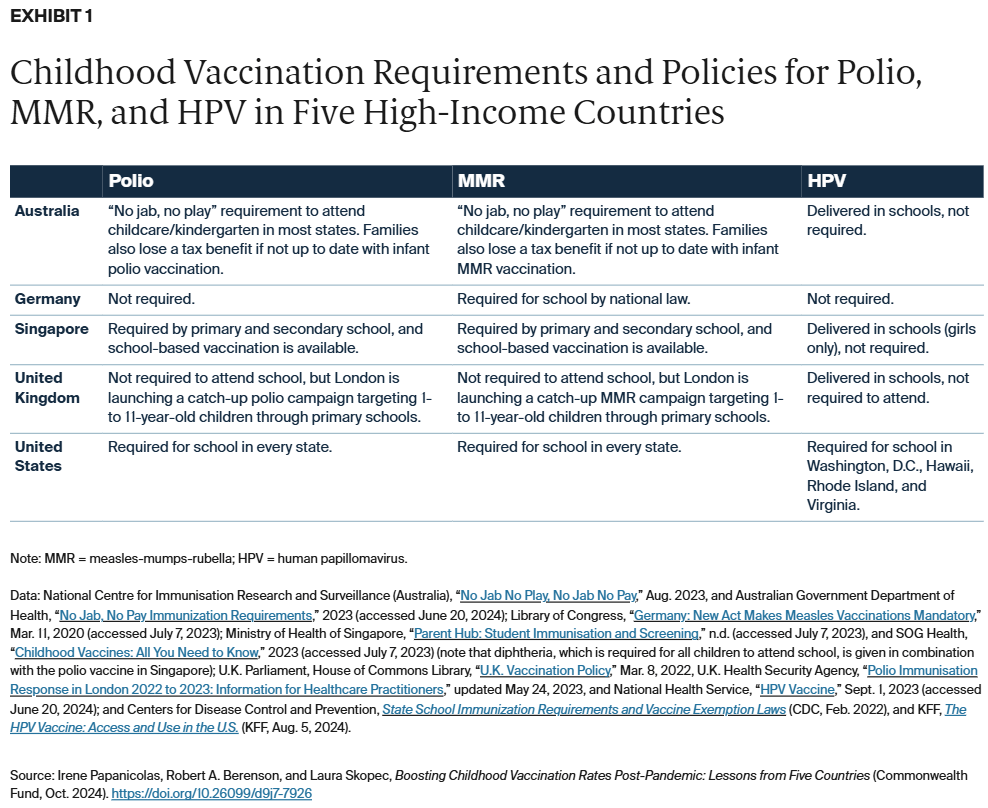

Among the countries studied, only Australia ties vaccination to financial incentives, requiring proof of polio and MMR vaccinations to receive child tax credits. In the U.K., in contrast, all vaccination is voluntary. However, to boost polio vaccination rates amid concerns about polio reemergence, London launched a voluntary catch-up campaign in primary schools in 2022 targeting children who did not receive the vaccine at the recommended age.8 In April 2023, the U.K. Health Security Agency announced that no polio isolates had been detected in wastewater since November 2022, suggesting transmission in London had been successfully reduced.9 This strategy suggests school-based vaccination could be an important route for improving vaccination rates.
HPV is not required nationally in any of the five countries, but Australia, Singapore, and the U.K. encourage vaccination by offering it for free in schools. Those three countries have far higher HPV vaccination rates than Germany and the U.S. (Exhibit 2), which do not offer school-based immunization. Only four U.S. states — Washington, D.C., Hawaii, Rhode Island, and Virginia — require HPV vaccination to attend school,10 but they do not offer free, school-based vaccine programs.
Changes in Vaccination Rates, 2018 and 2021
Polio vaccination rates fell in the U.S. and U.K. between calendar years 2018 and 2021 but remained steady in Australia, Germany, and Singapore (Exhibit 2). The share of 1-year-olds with one dose of the MMR vaccine also fell by 1 percentage point in Australia, the U.K., and the U.S. Shares of children who received two MMR doses by the nationally recommended age were more variable, however.
HPV vaccination rates rose in the U.S. and Germany, both of which had low rates pre-pandemic. In the U.K., however, HPV vaccination rates fell in 2021, though some of that decline reflects delays rather than failure to get vaccinated.11 Pandemic-related school closures, which varied substantially by country,12 may have disproportionately affected HPV vaccination rates in countries like the U.K. that offer school-based vaccination. HPV is the only vaccine in our study that is offered exclusively to school-age children.
Discussion
While vaccination rates fell worldwide during the COVID-19 pandemic, the high-income countries in our study, including the U.S., generally maintained high childhood vaccination rates for polio and MMR near or above the herd immunity threshold (80% for polio and 95% for measles).13 Australia and Singapore, which combine vaccine requirements with financial incentives (Australia) and school-based vaccination (Singapore), boasted the highest polio vaccination rates in both 2018 and 2021. The contrast between vaccination rates for polio and MMR in Germany, which requires vaccination for MMR but not for polio, also suggests that strong vaccination requirements may be instrumental in producing higher vaccination rates. However, it is unclear from this study if the observed pattern of higher vaccination rates for required immunizations in high-income countries would apply in low- and middle-income countries that had larger drops in vaccination rates during the pandemic.
Variations in HPV policies and vaccination rates also suggest that offering vaccines in school settings may increase uptake. Australia, Singapore, and the U.K. offer HPV vaccines for free in schools, and those countries have far higher HPV vaccination rates than Germany and the U.S., which do not offer free HPV vaccines in schools. Offering vaccines in school settings, perhaps combined with vaccine mandates, could be an effective strategy to boost lagging rates.14
In the U.S., vaccine hesitancy is a growing concern, especially in light of outbreaks of measles and cases of whooping cough and polio among children and young adults.15 Financial incentives, such as those used in Australia, could potentially increase vaccination rates — especially if they are paired with techniques to overcome hesitancy, including communication and community engagement from trusted sources like providers and community leaders.16 For school-age children, making it easier to obtain vaccines by offering school-based catch-up programs could also boost lagging immunization rates. Future research on the effectiveness of London’s school-based polio catch-up program would help policymakers determine if this strategy could also work in the U.S.17
This study has several limitations. First, our expert questionnaires and secondary data gathering were limited to a convenience sample of five countries. This study therefore does not represent a comprehensive picture of how vaccination policies and vaccination rates may vary across high-income countries. Second, because we gathered questionnaires from only two to four experts per country, we may have missed some within-country regional variations. Finally, we did not gather information on variations in vaccination rates by race or ethnicity or by other characteristics.
Conclusion
Variation in childhood vaccination rates among high-income countries may be related to differing approaches to immunization policy. This study highlights several promising policies for boosting vaccination rates that could be applied in countries that suffered drops in vaccination during the COVID-19 pandemic or have low vaccination rates for certain immunizations, like HPV in the United States. Such policies include offering vaccines in school settings and requiring parents to provide proof of vaccination to receive child tax credits.
Irene Papanicolas is currently an assistant professor of health economics in the Department of Social Policy/LSE Health at the London School of Economics. Check out Irene’s profile here
Laura Skopec is a senior research associate in the Urban Institute’s Health Policy Center, where her research focuses on health insurance coverage, health care access, and health care affordability. Check out Laura’s profile here
Robert Berenson is a senior fellow at the Urban Institute. He is an expert in health care policy, particularly Medicare, with experience practicing medicine. Check out Robert’s profile here
The original study is posted at Commonwealth Fund. Any reposting should credit the original author and provide links to both the GLP and the original article. Find Commonwealth Fund on X @commonwealthfnd