Next month, just as they did last year and the year before, researchers, doctors and public health officials collaborating with the World Health Organization will meet to decide what strains of influenza to include in the vaccine for the next season, 2015-16. And once this decision is made, the United States Vaccines and Related Biological Products Advisory Committee (VRBPAC) (a part of the Food and Drug Administration) considers the recommendations made by the WHO and decides upon the vaccine makeup for the US.
Then, in a process that hasn’t changed for decades, millions of of fertilized chicken eggs are injected with the chosen virus strains and allowed to grow inside the eggs before being purified to standards required by the FDA. This is the vaccine that eventually finds itself on product shelves. The whole process takes from six to nine months, which is why the strains to be included have to be decided well in advance.
One of the reasons that the flu virus has managed to survive so many of our attempts to thwart it is because of its ability to mutate at an amazingly fast rate, making any vaccine against it practically ineffective over the long run.
This makes the yearly exercise of selecting and producing a flu vaccine that is effective an unpredictable and frustrating affair. As you have probably heard in the news, this year was particularly bad as the CDC announced the results of their vaccine effectiveness study showing the seasonal flu vaccine was only 23% effective.
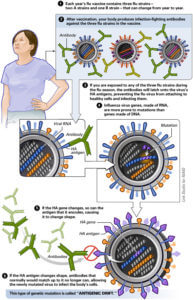
This is because the strain of the H3N2 virus that seems to be ravaging the country is one that ‘drifted’ from the strain that was included in the vaccine. Antigenic drifts, as they are called are small changes on the protein hemaggluttinin (HA) present on the surface of the virus which help the body detects its presence. The graphic below from the National Institute of Allergy and Infectious Diseases provides a great illustration of what antigenic drift is and why it reduces the effectiveness of the flu vaccine. (Another kind of change called an antigenic ‘shift’ changes the HA protein so that it creates a completely new virus subtype. Antigenic shift allowed the avian flu virus to jump from birds to humans in 2009, resulting in a pandemic)
Unfortunately, because rapid scale up is a practical impossibility with egg based production, we’re pretty much stuck with what’s been made already, severely limiting our response to this debilitating virus.
So this brings about the question, what can we do?
Quest for a ‘universal’ flu vaccine
Universal vaccines that need to be given only once are considered to be the holy grail against the influenza virus. Research efforts by scientists in both the private and public sector are attempting to create a universal vaccine by various approaches with the most significant one being a vaccine that that works around the mutation problem. This can be made possible by targeting vaccines against parts of the HA protein that don’t change much, as Sabrina Richards wrote in The Scientist
The answer to creating a vaccine that protects against many strains lies in forcing the immune system to make antibodies against the portions of the HA molecule that are shared, or genetically conserved, among most influenza viruses, thus creating a more universal vaccine. But, for unknown reasons, most vaccines don’t elicit such antibodies. So researchers are now trying new ways of enticing the immune system into making antibodies that recognize these general targets and neutralize many types of influenza at once.
Other methods to reate a univeral vaccine include selecting a target different from the HA protein on the viral surface or changing how the virus is delivered. But even if we do manage to make universal flu vaccines, there is a possibility tha tit may not last for a lifetime, as Sabrina Richards points out in The Scientist
Even if researchers do create vaccines that protect against all influenza viruses, we’ll still need to get vaccinated regularly—just not every year, said [influenza researcher at the University of Oxford Sarah Gilbert]. Unlike some other viruses, the flu doesn’t stimulate strong enough immune memory to keep us protected for life, even using a more universal vaccine. Gilbert estimates that future vaccines may stretch our yearly needle jabs to once every 5 years or so.
Not what we make but how we make it
Another alternative to making a better flu vaccine is to focus on not what we produce but how we produce it. The government has been funding several initiatives to identify faster methods of production that will essentially cut down the nine month waiting period for a vaccine.
Thus far, the FDA has approved two new technologies for vaccine production that do not rely on chicken eggs and makes production much faster. The first uses mammalian cells to produce the vaccine in large quantities. Approved in 2012, Novartis, the company that manufactured shipped the first full batch of the vaccine (called Flucelvax) in 2014. The second technology uses a genetically modified virus to produce a viral protein in insect cells. the protein is then purified and made into a vaccine, removing the need for any viruses in the vaccine itself. The vaccine produced using this technology, called Flublok was also made available for the first time this flu season.
Another promising technology that is emerging might also help change the fight against the flu. The tobacco plant which was the first plant to be genetically engineered has long used been used by researchers to produce proteins on a large scale. In the past few years, both biotech companies and the government have stepped up to the plate, using the technology to produce vaccines on a large scale.
For example, in a development that was widely publicized in the news in 2013, DARPA used genetically engineered tobacco to produce 10 million doses of avian flu vaccine containing specific viral proteins in just 4 weeks. More recently news that ZMapp the antibody based drug that is currently being tested for treating Ebola was produced in tobacco plants, has brought the technology back into focus. Small biotech firms such as the Canadian startup Medicago and Texas based Caliber Biotherapeutics are hoping to take their tobacco-produced flu vaccine to clinical trials soon. Universities such as Texas A&M are also researching the technology with support from the government, as Sharon Begley of Reuters writes,
“Seven to 10 years from now, plants might be the dominant vaccine-production system,” said Brett Giroir, an M.D. and CEO of Texas A&M Health Science Center in Bryan. Texas A&M has one of three U.S. facilities tasked by the government with being ready to produce and deliver 50 million doses of flu vaccine in just 12 weeks. It is working with Caliber toward that goal.
Despite the progress however, these technologies are yet to hit the mainstream market and we continue to rely on the tried and tested egg based production for the majority of our vaccine supply. One reason is because companies are hesitant to invest in a sector that has minimal financial incentives as Erika Fry points out in Fortune
Andrin Oswald, who heads the vaccine division at pharma giant Novartis, predicts we won’t reach the goal for another decade. “We haven’t seen an approach that makes us confident enough to invest,” he says.
And investment here is the key. In an age of $100,000 specialty meds, flu vaccines—which can be as cheap as $2 when demand is low—are not exactly a plum business. Even as the market has grown—in 2010, the CDC expanded its recommendation for a flu vaccination to everyone over the age of 6 months—the margins are thin. While Sanofi is exploring several universal flu vaccine strategies, Novartis is in the process of selling its money-losing flu vaccine unit—and a brand new $1 billion facility—to an Australian company for $275 million.
Accordingly, most innovation has been limited to incremental improvements to the annual flu vaccine—which can now be administered through a nasal spray or a skin patch and inoculate against four strains rather than three.
The influenza viruses is one of the smartest that our society has encountered, baffling scientists and doctors for almost a century. What if rather than trying to defeat the virus at the molecular level, we match the ability of the virus to mutate by getting our resources speeding up the vaccine manufacturing process? Getting all our eggs in the production basket may not be the best idea, but the current situation is equally imbalanced with a lot of the effort focussed on a universal vaccine. Balancing our baskets a little bit might lead to quicker rewards.
Arvind Suresh is a science communicator and a former laboratory biologist. Follow him @suresh_arvind
Additional Resources
- What goes into the flu vaccine?, Wired
- Gut microbiome makes flu vaccine more or less effective, The Scientist
- Are flu shots effective? Your genetics determine how the immune system responds, Genetic Literacy Project