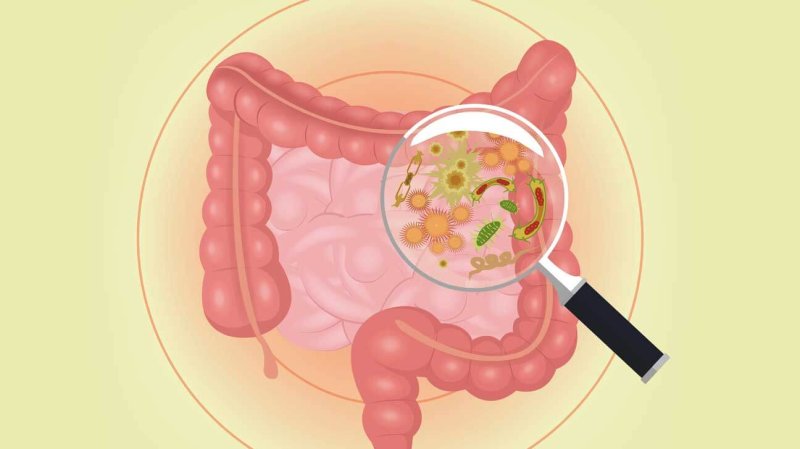
It’s so common the CDC estimates 30 to 70 percent of travelers are affected, depending on where they go. Most cases are caused from food or water contaminated with locale-specific bacteria. Those bacteria cause the adverse reaction in our guts. They can also carry antibiotic resistance genes. And it turns out we can pick up those bugs very quickly—just 48 hours according to new research presented at the American Society for Microbiology meeting.
Antibiotic resistance genes are a big problem. A recent report found that sexually transmitted infection, gonorrhea, is developing resistance to the last two antibiotics that treat it. Because bacteria can share genetic information between themselves in a processes called horizontal gene transfer, they can acquire resistance genes quite quickly. Resistance genes are specific to a particular drug or drug family, explains David Cox at the Guardian:
At the molecular level, such mutations can prevent an antibiotic entering the bacteria cell at all, altering the target molecules so that they don’t bind to the antibiotic anymore, or enhancing the efficiency of efflux mechanisms within the bacteria which allow it to simply pump a drug back out again. Certain genes, if acquired, can actively degrade antibiotics, limiting their effectiveness once they’ve entered the cell.
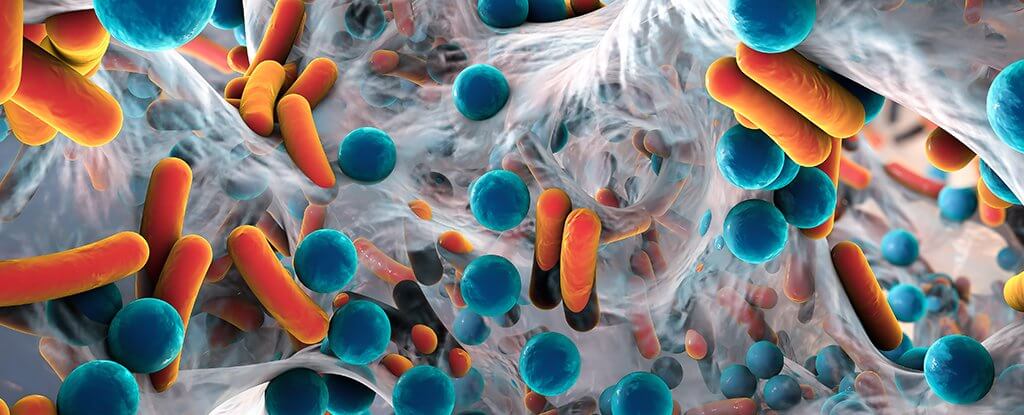 Petra Wolffs and her colleagues discovered genes picked up by the bacteria in the traveler’s guts depended on where they went on vacation. Quinolone-resistance genes were most common among travelers returning from India where the drug is manufactured, incidentally. From Andy Coghlan at New Scientist:
Petra Wolffs and her colleagues discovered genes picked up by the bacteria in the traveler’s guts depended on where they went on vacation. Quinolone-resistance genes were most common among travelers returning from India where the drug is manufactured, incidentally. From Andy Coghlan at New Scientist:
Within two days of reaching India, for instance, two travellers had picked up qnrB, a gene that makes bacteria resistant to quinolone, one of the world’s most important antibiotics. The travellers’ gut flora retained the new genes for at least one month after they had returned home.
In a previous study, Wolffs found that almost all travelers had gut bacteria resistant to tetracycline, a very common antibiotic, even before they left the Netherlands. That may suggest that travelers themselves are spreading resistance genes in the communities they visit.
Getting sick from eating exotic foods while abroad is common and to some extent expected. But even if a traveler drinks only bottled water, forgoes ice and fruits without peels, she can’t completely eliminate the chance of contamination. Foods, dirt, animals, water and even other people are often contaminated with microscopic bits of fecal material that are largely unavoidable, according to Drake Baer at New York Magazine:
Not that you should be extremely worried about all that poop… Because if there aren’t any pathogens in a given feces, he says, “you can spoon-eat feces without any deleterious effect.” While the world may be “covered in a fine patina of feces,” as one Stanford microbiologist observed, you’re mostly okay unless there are pathogens in there.
So are these resistance carrying gut bacteria going to make us sick? It’s not likely says Wolffs. The small numbers of acquired resistance-carrying bacteria are dwarfed by the mammoth numbers of a traveler’s normal (native at least to the individual) gut flora. Unless there is something exceptionally aggressive about the resistance-carrying bacteria they are unlikely to sway the balance of the gut flora and make travelers ill. In Wolffs’ studies, the resistance-genes couldn’t be found after a couple of months. The organisms that carried them simply died off in the natural turnover of the gut microbiome.
But for some travelers, even small, sporadic exposures might contribute to illness. Travelers with compromised immune systems or those with chronic diseases like diabetes are more susceptible to infections, in general. These groups also pick up resistant infections more than a normal, healthy population.
Wolffs’ research will next track traveler’s returning home to see if they can spread the resistance-carrying bacteria picked up abroad to friends and family. If so, that would further the case that international travel is an important factor in spreading antibiotic resistance and a possible target for interventions to contain resistance genes after a trip. Hopefully, research in this vein will yield some effective strategies to avoid a global antibiotic-resistance pandemic.
Meredith Knight is a frequent contributor to the Genetic Literacy Project. She is a freelance science and health writer based in Austin, Texas. Follow her on Twitter @meremereknight.