The diversity of medical conditions in crowdfunding campaigns for stem cell treatments reflects the perception that stem cells can cure anything. Indications range from the common – stroke, autism, multiple sclerosis, to Parkinson’s disease – to genetic diseases, injuries, degenerative conditions, and even infections. Yet some people seek stem cell support for “a fresh lease on life” or “rejuvenation.” More common, though, are tragic narratives of a “last option” or “a few months left.” They’re hard to read.
The issue of unapproved treatments was thrust into the public’s eye with the recent announcement by the FDA that it is seeking to stop a pair of clinics — one in Florida and another in California — from selling stem cell therapies after patients were blinded. At the heart of the issue are FDA regulations that dictate which types of stem cell interventions are not illegal to provide, even if they are not specifically agency-approved for marketing. So it’s complicated. The case of the blinded-by-stem-cells patients was extreme in that it transferred stem cells cultured from their abdominal fat (removed by liposuction) into their eyes — a highly unnatural intervention that goes against the regulations.
Companies can consult FDA regulations to determine which applications of stem cells do not require the agency’s approval for marketing.
A stem cell can divide to yield another stem cell (“self-renewal”) and a cell that can differentiate (specialize). The self-renewal is critical to not using up the precious cells. Stem cells might heal by giving rise to differentiated cell types like neurons, or by secreting growth factors or other proteins. They may replace ravaged cells and perhaps sooth others. Bone marrow is a rich source of stem cells.
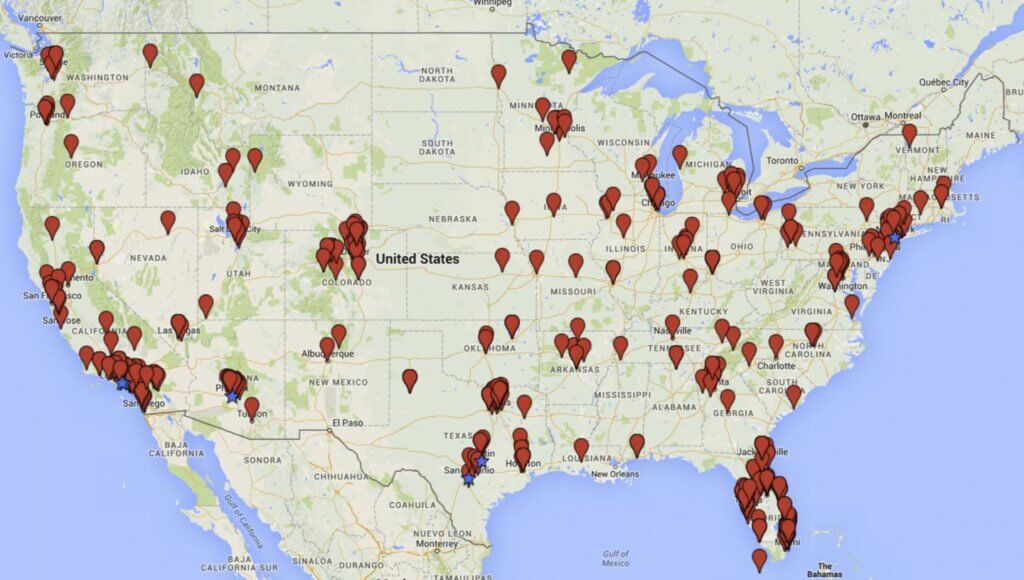
Crowdfunding campaigns may be short on technical details yet overstate efficacy, based on information from direct-to-consumer stem cell company websites. Jeremy Snyder, PhD, and Valorie A. Crooks, PhD of Simon Fraser University in British Columbia, and Leigh Turner, PhD, from the University of Minnesota, recently published “Crowdfunding for Unproven Stem Cell–Based Interventions” in the Journal of the American Medical Association. They found 50 campaigns on YouCaring and 358 on GoFundMe, searching with the names of 351 companies identified in a 2016 study, “Selling Stem Cells in the USA: Assessing the Direct-to-Consumer Industry” published in Cell Stem Cell.
The 408 crowdfunding campaigns overall sought $7,439,308, with $1,450,011 contributed from 13,050 donors, and 111,044 social media shares. The investigators rated the degree of confidence in efficacy of the sought-after treatment. Of the 408 campaigns, 43.6% (178) made “definitive or certain” statements about efficacy, 30.4% (124) were “optimistic or hopeful,” 15.4% (63) “definitive and optimistic,” but only 10.5% (43) didn’t claim efficacy.
Only 36 of the campaigns mentioned risks, but that’s understandable, said Dr. Turner. “Individuals who have created these campaigns are hoping to obtain donations for procedures they believe will help them. They’re focused on creating compelling narratives that will convince friends, neighbors, and strangers to donate to them, and on the therapeutic benefits that they hope will result from the stem cell interventions.”
Cases
The new paper is only a page and doesn’t mention specific crowdfunding campaigns, but they’re easy enough to find.
The case of a guitarist for the band Snot is classic. He suffered two heart attacks at an age young enough to suggest a strong genetic predisposition, which he acknowledges, and then states that heart disease is “absolutely preventable through diet and lifestyle,” which presumably the rockstar lifestyle failed to provide. He says he has done research that convinced him that mesenchymal stem cells (MSCs) are the way to go. His page cites this article as evidence of efficacy. It reviews studies demonstrating how MSCs can fight heart disease — but nearly all of them are in mice.
Another case: Ron. He posted in 2015, when he was seeking $21,600 to be part of the Stem Cell Ophthalmology Treatment Study (SCOTS), a clinical trial offered by MD Stem Cells to stop or reverse a number of eye conditions, including his Stargardt’s disease, which causes blindness from macular degeneration.
SCOTS also enrolls people with retinitis pigmentosa, age-related macular degeneration, Ushers syndrome, glaucoma, ischemic optic neuropathy, Lebers hereditary optic neuropathy, and a variety of optic atrophies (degenerating eyes) from injury, inflammation, toxins, or autoimmunity. “We’re interested in optic nerve or retinal disease that is on a cellular basis. Macro changes such as a retinal detachment aren’t eligible,” said Steven Levy, MD, study director at MD Stem Cells. The stem cells, from the patient’s own (autologous) bone marrow, are injected behind the eyeball and also given intravenously. These stem cells naturally home to the circulation and the brain.
Ron would be part of Arm 3 of the clinical trial, which is seeking 500 participants. The trial is open-label and non-randomized – that is, no controls, such as an untreated group. But that’s common for clinical trials for rare diseases, in which treated patients are compared to natural history studies that track the course of an untreated illness.
Patients must travel to the Fort Lauderdale area for a 3-day stay, after clearance by their primary care physician.
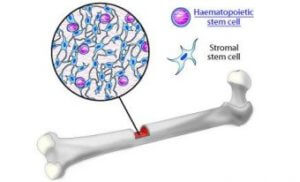
Bone marrow retrieval isn’t cheap. The $19,600 “includes preoperative examination and testing, examination and testing for 6 months postoperatively, four MDs involved in various stages of the study, all surgery center fees including anesthesia, and the FDA-approved machines and disposable packs used to separate out the stem cells,” said Dr. Levy. Travel costs are extra.
Ron’s GoFundMe page quotes from Dr. Levy: “There are three groups of treatments or arms of the study which may be reviewed on the NIH website.” And the company’s website refers to “NIH registered studies.”
Might a patient infer that the NIH has sanctioned the trial, rather than just it’s listing at ClinicalTrials.gov? I can sell a spittoon on Craig’s List without being a professional antiques dealer.
Typically the NIH, a pharmaceutical company, or a not-for-profit such as a parent-run foundation funds a clinical trial. “In most clinical trials, study subjects are not charged fees to participate. In contrast, individuals enrolled in what are often called ‘pay-to-participate’ studies are charged thousands or tens of thousands of dollars. … some businesses are using the ClinicalTrials.gov registry to promote stem cell interventions that study subjects are charged to receive,” wrote Dr. Turner in Regenerative Medicine in September 2017.
Evidence of efficacy
MD Stem Cells’ website says that the company “provides the only stem cell treatments in ophthalmology with medical journal published, statistically significant results.” The studies are indeed in peer-reviewed journals, but claims of statistical significance seem to refer to the measures of improved vision, and not (yet) to the numbers of patients. The investigations are small.
A study from 2017 of 10 patients, 8 of whom did well, for non-arteritic ischemic optic neuropathy, lead to the company’s claim that “In our report there was statistically significant visual improvement for a sizable majority (80%) of patients, with over 73% of individual eyes benefitting from the treatment.” Percentages on a sample size of 10 patients/20 eyes seems odd.
In a case report from 2015, a young woman who lost her vision over a few weeks due to an undiagnosed form of optic neuritis dramatically improved after stem cell treatment, from 20/800 in the right eye and 20/4000 in the left, to 20/100 in the right and 20/40 in the left. A second case report was published in 2015 too, and another in 2016. Findings on 5 patients with Leber’s hereditary optic neuropathy were also published in 2016.
A soon-to-be-published study will add 17 patients (33 eyes) treated for retinitis pigmentosa, said Dr. Levy. Eleven patients had improved binocular vision while 6 remained the same.
That’s a total of 35 patients followed in the reports, but hundreds have been treated, according to the company website. I wonder how many have been treated and disappointed. A controlled clinical trial that proceeds through phase 3 would provide that type of information.
Despite the small samples, the findings are promising. But the company is careful. On the opening webpage, beneath the mention of statistical significance in good journals and “scientifically proven results” is, just a click away, a DISCLAIMER: “The stem cell studies available through MD Stem Cells are Institutional Review Board (IRB) approved and FDA compliant. They are open label, non-randomized efficacy studies and no guarantees of specific results or improvements to participating patients are being made.”
So all is transparent if a potential patient reads the disclaimer and understands the workings of ClinicalTrials.gov and the FDA. Delving into the actual FDA regulations reveals that companies can indeed provide certain types of stem cell procedures. And changes afoot at the agency may encourage small stem cell companies to pool data, perhaps finally building the numbers to get FDA approval and insurance companies on board for more treatments.
 View From the FDA
View From the FDA
In March 2018, Peter Marks, MD, PhD and FDA Commissioner Scott Gottlieb, MD, published in The New England Journal of Medicine “Balancing Safety and Innovation for Cell-Based Regenerative Medicine.” Their goal: to ease the identification of stem cell treatments that work.
The FDA considers stem cells part of regenerative medicine. The Public Health Service Act includes them among the “HCT/Ps” – “human cells, tissues, and cellular and tissue-based products.” Sections 351 and 361 then divvy up stem cells into two groups.
Section 351 lists specific products that FDA regulates: a “virus, therapeutic serum, toxin, antitoxin, vaccine, blood, blood component or derivative, allergenic product, or analogous product, … applicable to the prevention, treatment, or cure of a disease or condition of human beings.”
Section 361 doesn’t mention cell types, but says FDA can regulate a product for ability to spread infection. So if a variety of stem cell doesn’t fall under 351, then all it has to be is infection-free to inject it into a patient.
But in 2005 came a critical change. The Code of Federal Regulations part 1271 of Title 21 fleshed out description of cells under section 361, affecting the offerings of stem cell companies. Cells should be:
- minimally manipulated
- have the same function in the body (so no tummy fat injected into the eyes)
- free of another drug or biologic
- have a localized (not systemic) effect
- not require metabolism to activate them
The fat-to-eye transfers in the Florida clinic violated the first two criteria: the cells were manipulated and did not end up where they would in a healthy human body. But according to part 1271, things like skin, amniotic membrane, sperm, tendons, heart valves, and corneas just need to be listed with the FDA. There’s no requirement for an investigational new drug or biologics license application following clinical trials. Gene therapies, targeted cancer drugs, cultured nerve and cartilage cells, stem cells from non-relatives — all must traverse the FDA labyrinth to market approval. But not some stem cells, like those from a patient’s own body that go to a place they normally would.
More recently, the FDA announced a regenerative medicine advanced therapy (RMAT) designation to catalyze investigations if preliminary clinical evidence indicates targeting an unmet medical need for a serious or life-threatening condition. Plus, the RMAT can include “traditional studies as well as the submission of patient registries or other sources of real-world evidence,” Drs. Marks and Gottleib write. So the patients who pay for their treatments may ultimately speed the FDA approval that insurers seek.
In November 2017, the FDA released a comprehensive framework for oversight of regenerative medicine to help companies distinguish which stem cell applications require pre-market approval. Part of the framework is to encourage small groups of physicians to develop clinical trial protocols to test treatments, manufacturing their own products and delivering them, then pooling data. If the treatment is safe and efficacious, then FDA would provide a biologics license to each group, providing incentive and lessening the need to seek funding from pharma or from crowdfunding.
Sums up Dr. Turner:
From a regulatory perspective crowdfunding sites could serve as an investigative gold mine. But then one reason hundreds of U.S. businesses are selling unproven and unlicensed stem cell interventions is that the FDA has paid insufficient attention to this marketplace. The FDA’s commissioner, Scott Gottlieb, has made some encouraging remarks about increased enforcement efforts but to date I haven’t noticed a reduction in the number of businesses, misleading advertising claims, or crowdfunding campaigns established by individuals targeted by these clinics.
In the meantime, patients who turn to crowdfunding may find hope, perhaps tempering the feeling of helplessness that builds as symptoms worsen. Although Dr. Turner is critical of companies that oversell their stem cell products and finds the crowdfunding pitches disturbing, he understands the desperation. “We’re all an illness or accident away from joining their ranks, assuming we’re not already among them.”
Ricki Lewis is the GLP’s senior contributing writer focusing on gene therapy and gene editing. She has a PhD in genetics and is a genetic counselor, science writer and author of The Forever Fix: Gene Therapy and the Boy Who Saved It, the only popular book about gene therapy. BIO. Follow her at her website or Twitter @rickilewis.