In fact, they couldn’t have been more wrong. Thinking that a novel virus is exactly like a familiar one is like assuming that a guinea pig is the same as a rat.
The confusion arises from using “flu” to denote the familiar litany of respiratory misery, fever and fatigue. These symptoms are mostly due to the response of the immune system to infection. But the specific illness “influenza” is actually due to infection from an influenza virus (not to be further confused with the tiny bacterium Hemophilus influenza).
The Director-General of the World Health Organization (WHO), Tedros Adhanom Ghebreyesus, puts it succinctly. “This virus is not SARS, it’s not MERS, and it’s not influenza. It is a unique virus with unique characteristics.”

The early comparisons to influenza led some people to suggest administering flu vaccines to ward off the new virus, SARS-CoV-2. But a vaccine is created to fit a specific part of the topography of the targeted pathogen. You wouldn’t wear a hat on a foot.
Here are the similarities and differences between the two pathogens, with focus on influenza A, the most prevalent one that makes us sick.
Similarities
Neither influenza A nor SARS-CoV-2 respond to antibiotics, which treat bacterial infections.
A virus is simply a genome (of DNA or RNA) inside a protein coat with perhaps attached sugars and a fatty envelope. Too streamlined for biologists to consider them to be alive, viruses reproduce only if they commandeer a host cell’s energy resources, protein synthetic machinery, and pathway to secretion.
Influenza A and SARS-CoV-2 each have RNA as their genetic material, along with RNA polymerase to continually make more RNA. Lots of viruses are RNA-based: those that cause colds, hemorrhagic fevers like Ebola and Marburg, hepatitis, AIDS, rabies, dengue and yellow fever. They’re notorious for mutating rapidly and not repairing the errors.
Both influenza and COVID-19 cause fever, cough, respiratory symptoms — including pneumonia — body aches, fatigue, and sometimes vomiting and diarrhea. Severity ranges greatly for each.
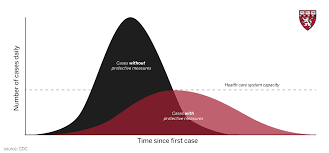
The number of cases is fast becoming similar for the two viruses. COVID-19 has yet to really ramp up, but may reach influenza levels: 9.3 million to 45 million cases and 12,000 to 61,000 deaths in the U.S. per year. Already cases of COVID-19 are significantly higher than for SARS and MERS, which are also caused by coronaviruses but are not transmitted as readily as the newcomer.
Influenza A and COVID-19 are each spread through droplets in the air from an infected person coughing, sneezing or talking, or through presymptomatic or even asymptomatic carriers. The novel coronavirus persists in aerosols (smaller than droplets) for hours and on surfaces for days, but it isn’t yet known how much virus on various fomites – things in the environment – is required to make people sick.
For both influenza and COVID-19, treatment is supportive. That means “maintaining fluid status and nutrition and supporting physiological functions until we heal. It’s treating complications and organ support, whether that means providing supplementary oxygen all the way to ventilator support, and just waiting it out. If a patient progresses to acute respiratory distress syndrome, it becomes tougher,” infectious disease specialist David Liebers, MD, chief medical officer at Ellis Medicine in Schenectady, New York, told me after he’d put in a 14-hour day last week.
Both influenza and coronaviruses have been around awhile, although SARS-CoV-2 is indeed novel and that’s why no one is immune to it.
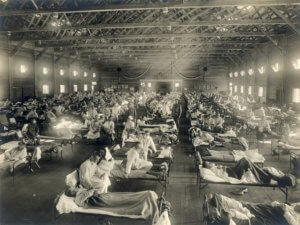
The first influenza virus was isolated in 1933, although of course by then the world was familiar with it from the 1918 pandemic. Flu viruses are thought to have arisen about 6,000 years ago.
The first two of the seven (of 39 recognized) coronaviruses to infect humans were discovered in the 1960s. They cause about a third of colds (upper respiratory infections) and some cases of pneumonia in people with weakened immune systems.
In 2002 came Severe Acute Respiratory Syndrome – SARS – with more than 8,000 infections and 774 deaths. Another human coronavirus described in 2004 causes pneumonia and bronchitis, rarely, but most of us have antibodies to it, indicating past exposure that didn’t make us very sick. In 2005 came yet another, causing pneumonia in young children and respiratory distress syndrome in adults.
MERS (Middle Eastern Respiratory Syndrome) emerged in 2012 in the Arabian peninsula, and is rare but can be fatal. SARS and MERS show zoonotic (to other animals) as well as human-to-human transmission.
Both influenza A and coronaviruses are zoonotic, “spilling over” from one animal species to another. (“From animals to humans” makes no sense; we are animals too.)
Differences
Like the guinea pig and rat, influenza virus and SARS-CoV-2 aren’t much alike.
Influenza comes from birds, sometimes passing through pigs, horses, camels, or seals.

Coronaviruses come from bats, sometimes passing through other “reservoir” species. The fact that SARS-CoV-2’s genome most closely matches that of a bat coronavirus and a Malayan pangolin virus suggests that bat-pangolin-person may have been the trajectory – the jury is still out on the origin.
Both influenza and coronaviruses have a single strand of RNA as the genetic material. But SARS-CoV-2 is “positive sense,” which means that the infected cell can use it as is, recognizing the viral RNA as its own messenger RNA and being fooled into cranking out viral proteins. An influenza virus is “negative sense,” which means that a cell first has to copy it into a complementary form, as RNA is normally transcribed from DNA.
Taxonomically speaking, SARS-CoV-2 belongs to family Coronaviridae and influenza A to family Orthomyxoviridae. Guinea pigs and rats are rodents that belong to different families, which is the level above genus, which is above species.
Classification of viruses is tricky.
While the WHO has traditionally named viral diseases according to places, times, and host species, that’s been deemed stigmatizing, such as the “Spanish flu,” 1918 pandemic, and swine flu. The International Committee on Taxonomy of Viruses (ICTV) classifies viruses based on genome sequences.
The genomes of influenza viruses and coronaviruses include the same basic tools to make RNA, package themselves, and burst forth from infected host cells. Beyond that, they’re different.
At 29,811 bases, the newbie’s genome is about twice the size of influenza A’s, which is 13,588 RNA bases.
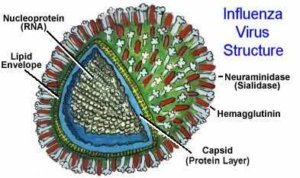 The genome of influenza A consists of 8 RNA segments that encode 12 proteins. The viral surface sports two types of glycoproteins, hemagglutinin (HA) and neuraminidase (NA). HA comes in sixteen varieties and NA in nine, generating much of the diversity of the virus, as well as the names of the strains. The 1918 “Spanish flu” and the “swine flu” of 2009 were “H1N1,” whereas the “bird flu” of 2004 was “H5N1.”
The genome of influenza A consists of 8 RNA segments that encode 12 proteins. The viral surface sports two types of glycoproteins, hemagglutinin (HA) and neuraminidase (NA). HA comes in sixteen varieties and NA in nine, generating much of the diversity of the virus, as well as the names of the strains. The 1918 “Spanish flu” and the “swine flu” of 2009 were “H1N1,” whereas the “bird flu” of 2004 was “H5N1.”
The HA parts of influenza viruses bind to sugars on respiratory cell surfaces, called sialic acids, that serve as the viral receptors, or doorways. A “flu” is a respiratory infection. This is why vomiting on a cruise ship from a norovirus infection is gastroenteritis, not “stomach flu.”
SARS-CoV-2’s genome encodes 16 enzymes required to make viral parts plus four “structural” proteins that build the virus’s distinctive form.
“S” protein makes up the spikes that festoon the coronaviruses and gave them their royal name. Three identical S proteins form each spike, and the spikes grab the receptors – which aren’t the same as for influenza A. The identity of a virus’s receptor is the very crux of how their associated illnesses differ clinically, because it dictates where the immune response begins, which affects the choreography of the unfolding of symptoms.
The receptor for SARS-CoV-2 is ACE2, found on human cells of the lower lungs, in the upper respiratory passages, and in some blood vessel linings. Beneath and around the spikes, nucleocapsid proteins knit a layer of identical subunits, like the panes of a greenhouse, cloaking the virus from our immune system’s interferons and from RNA interference.
 Many unknowns
Many unknowns
We can’t yet accurately compare the fatality rates of influenza A and COVID-19, or even calculate it for the new virus, and likely won’t be able to until antibody tests reveal people who had mild cases of the novel infection or were asymptomatic. The mortality rate for influenza in the US is under .1 percent; initial estimates for COVID-19 peaked at 3.2% during the pandemic’s infancy in China.
Complicating diagnosis of respiratory symptoms is that a person can be infected with both influenza and COVID-19. Not testing patients for COVID-19 because they initially test positive for influenza, then, can miss the dually infected.
That’s what happened to a 69-year-old who tested positive for influenza A at the China-Japan Friendship Hospital, was admitted, and discharged days later after he improved. When he worsened and returned, a CT scan revealed “ground glass” opacities in his lower lungs, a telltale sign of the novel coronavirus. His saliva and throat samples were still negative for SARS-CoV-2, but his lung fluid was positive.
So we still have a lot to learn.
We don’t yet know how changeable the novel coronavirus is. An early estimate of the mutation rate is 2 RNA bases a month. With time, that could spawn a stream of viral variants, but whether that would affect the severity of illness isn’t known.
The changeability of influenza viruses is obviously much better understood and partly explains why vaccines can be ineffective. These viruses are shape shifters. They “drift” modestly when single RNA bases change, and “shift” dramatically when different viral strains swap hunks of themselves in different creatures, generating a zoonose. The 2009 H1N1 flu pandemic arose from a viral square dance of sorts in the throats of North American and Eurasian pigs.
Individual immune responses to SARS-CoV-2 are another unknown. Some people have minor symptoms, like Tom Hanks, while others die quickly from an overactive immune response called a cytokine storm. (See “Two Women Fell Sick. Only One Recovered,” which dispels the idea that only the older and ill contract COVID-19.)
I’ve long been utterly fascinated with viruses. The relationship between viruses and humans can seem like a science fiction plot.
The viruses that make us sick may be little more than snippets of genetic material borrowed, long ago, from human genomes. Wrapped in fat also sampled from our cells, viruses return to us, binding to molecular doorways on our cell surfaces, invading, taking over to make more of themselves, and bursting forth. They may not be alive, but the viruses can be formidable enemies of humanity.
Ricki Lewis is the GLP’s senior contributing writer focusing on gene therapy and gene editing. She has a PhD in genetics and is a genetic counselor, science writer and author of The Forever Fix: Gene Therapy and the Boy Who Saved It, the only popular book about gene therapy. BIO. Follow her at her website or Twitter @rickilewis































