The president denied these claims, but the outcry highlighted the high regard in which the American public, and most of the world, holds veterans; people are united by the pride and respect for those brave enough to risk life and limb for their country.
In the United States, the number of injured soldiers returning home alive has risen from 75% to 92% since the Vietnam War, but combat takes a toll on the survivors. It’s estimated that one in every 10 veterans alive today was injured seriously while serving. And, for many, the nature of the injury makes treatment very difficult. Soldiers can find themselves returning home with severe burns, spinal cord injuries, paralysis, blindness, deafness, brain injuries and loss of limbs, as well as psychological trauma, some linked directly to physical injuries.

Regenerative medicine breakthroughs address bone complications
The most significant development in recent years for severely maimed veterans and other victims of physical injuries is the acceleration of what’s known as regenerative medicine. Regenerative medicine was first defined in 1999 and it encompasses many disciplines of science. Its goal is to provide clinicians with the tools to effectively repair or replace a patient’s damaged tissues and organs in order to return normal function.
The technology really emerged into the public consciousness in the 2000s because of the Iraq war and, since then, great strides have been made in applying it to treating many different healthcare issues. So, what about the specifics? What are the most promising breakthroughs in recent years?
Some of the most challenging war-related injuries involve bones. Severe burns, spinal cord injuries, blast injuries, traumatic brain injuries—these seemingly disparate traumas can each lead to a painful complication during the healing process called heterotopic ossification (HO).
A team at Michigan Medicine’s Department of Surgery is focusing its research on how the healing process often goes awry. The problem often emerges at limb amputation sites. Weeks after surgery or injury, abnormal bones often form within soft tissues like muscle—places where they’re not supposed to be, causing the patient agonizing pain.
“There’s no way to prevent it and once it’s formed, there’s no way to reverse it,” said Benjamin Levi, M.D, co-head of the research team at the Center for Basic and Translational Research at Michigan Medicine’s Department of Surgery.
There may be a solution thanks to a collaborative study between Levi and a research group led by Stephen Kunkel, Ph.D. at Michigan’s Department of Pathology. It had been theorized that HO could be linked to inflammation at the site of injury or surgery. The researchers built on this theory by studying the cells that are present at the early stages of HO.
Working with mice, they have been able to identify a specific protein that is responsible for sending the signals that trigger stem cells within the bone to start this process of uncontrolled tissue growth. By targeting this protein and stopping its action, it could be possible to stop the process in the first place. This would improve the quality of life for many injured veterans.
Treating HO is very much a case of prevention being better than cure. Progressing this discovery into a therapeutic setting could eventually provide doctors with a mechanism to stop HO before it has a chance to develop. It would be a game changer for many veterans who would otherwise be left with this agonizing condition.
Prosthetics
Severe blast injuries and bullet traumas also leave many veterans needing implants or prosthetics to replace bone that has been lost to severe injury. If you break a leg, a doctor will put it in a cast and allow the natural healing process to occur. If it’s a severe break, you may need surgery. But when a soldier’s bone is ripped apart by a gunshot or a blast, the damage to the network of cells within the bone is so severe that it often cannot heal on its own.
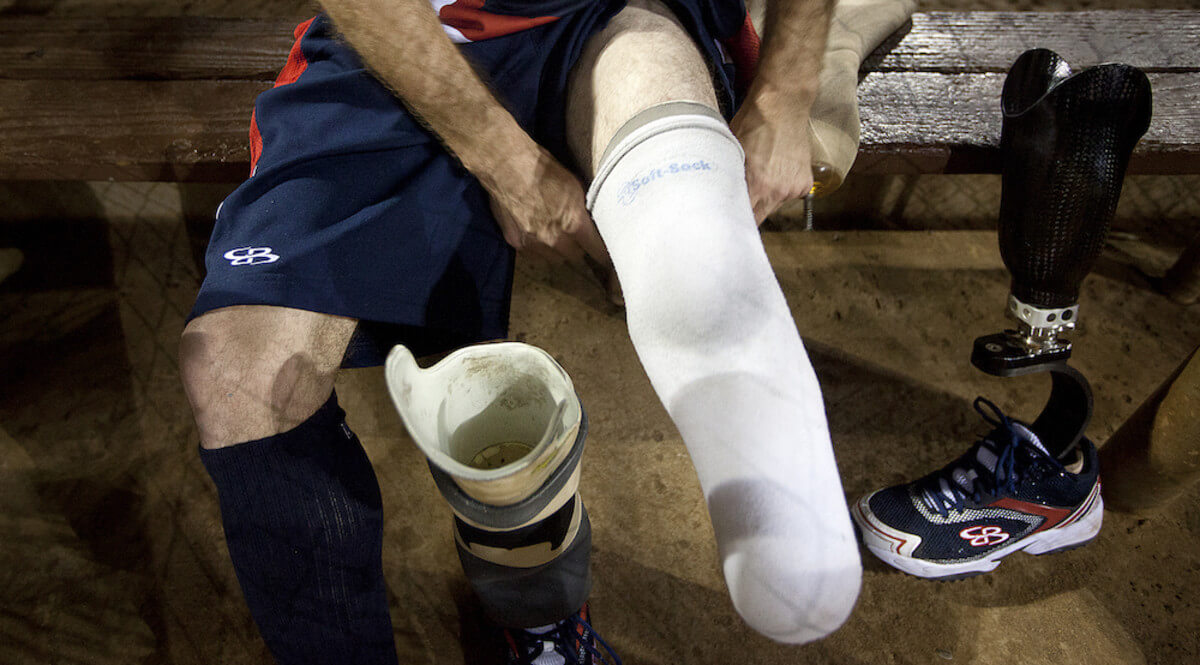
Regenerative medicine may provide a solution. After leaving the US Army more than 20 years ago, solider Luis Alvarez founded a firm at the Massachusetts Institute of Technology that developed a “paint” derived from key proteins that can trigger bone regeneration. The inspiration behind Alvarez’s innovation?
During my time in Iraq, I witnessed service members who suffered traumatic injuries undergo amputations weeks or months after the initial wound, because there was no reliable method for regenerating the bone.
The technology developed by his company allows doctors to coat implants with specific proteins, allowing them to trigger regeneration, thus aiding recovery of the damaged tissue. They are making great progress and looking to have something ready for doctors to use in clinics by 2021. It’s an inspiring story. The company is rolling out multiple therapies heading into clinical trials over the next two years.
Bioprinting
The military is also starting to invest heavily in one of the most exciting avenues of regenerative medicine to help veterans replace lost tissue. Bioprinting uses human cells mixed with specially designed “bioinks” to 3D print tissue-like structures for the purpose of regenerating damaged body parts. Using bioprinting, scientists can build replacement grafts using a patient’s own stem cells, thus removing the issues associated with transplant rejection. The technology is still in its infancy but, thanks to recent military investment, scientists are now applying bioprinting to the generation of skin grafts to treat the severe burns that many veterans are afflicted with.

Treating severe burns is an incredibly difficult process and many rarely heal completely. Patients can be left with extreme scarring, tight and itchy skin and disfigurement. When the skin is severely burned the body focuses on preventing infection by closing the wound as quickly as possible. New skin is generated but the structure is vastly different to “normal” tissue.
A 5-year research project led by Prof Jeff Biernaskie at the University of Calgary Faculty of Veterinary Medicine has made a big step forward.
What we’ve shown is that you can alter the wound environment with drugs, or modify the genetics of these progenitor cells directly, and both are sufficient to change their behaviour during wound healing. And that can have really quite impressive effects on healing that includes regeneration of new hair follicles, glands and fat within the wounded skin.
This research could lead to new drugs that greatly improve the healing process.
It is clear from the number of veterans currently coping with a compromised quality of life that we need to do more to treat their injuries. It is estimated that the number of veterans currently living with these life changing injuries is in the millions and their healthcare needs come at an immense economic cost. Fortunately, there is now a much stronger horse in the race to a cure.
Regenerative medicine was estimated to draw nearly $15 billion in investments in 2017. That figure is predicted to rise to in excess of $79 billion by 2026. Those are serious resources, providing hope that our veterans will benefit in the decade ahead.
Sam Moxon has a PhD in regenerative medicine and is currently involved in dementia research. He is a freelance writer with an interest in the development of new technologies to diagnose and treat degenerative diseases. Follow him on Twitter @DrSamMoxon