In the words of researcher He Jiankui, of Southern University of Science and Technology in Shenzhen:
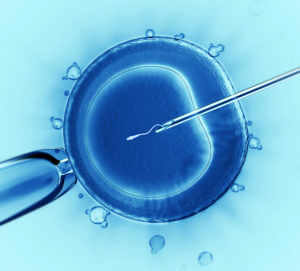
Two Chinese girls, who we’ll call Lulu and Nana to protect their privacy, were born healthy a few weeks ago. Their mother Grace started her pregnancy by regular IVF with one difference: right after sending her husband’s sperm into her eggs, an embryologist also sent in CRISPR/Cas9 protein and instructions to perform a gene surgery intended to protect the girls from future HIV infection. The surgery reproduces a natural genetic variation shared by more than 100 million people of primarily European origin that confers strong resistance to initial HIV-1 infection and disease progression.

Dr. He went on to briefly explain the safety measures taken: genome sequencing before the early embyros implanted in the uterus, during the pregnancy, and after birth. “These data indicate the girls’ genomes were changed as intended by the gene surgery, but no off-target editing or large deletions occurred,” he concluded, saying his team would publish the findings soon.
Condemnation was swift and relentless, reverberating through the news media, with co-CRISPR-inventors and various other luminaries of science chiming in. The American Society of Human Genetics quickly reaffirmed its 2017 Position Statement on Germline Genome Editing, with president David Nelson adding in a news release:
It is premature to perform germline genome editing that culminates in human pregnancy. Important scientific, ethical, and policy discussions are taking place, but many vital questions remain unanswered.
In other words, manipulating human eggs, sperm, and embryos might be ok, but only if the nurturing ensues in laboratory glassware. For now.
A few days later, on December 3, the debate hadn’t simmered down. Director-General Tedros Adhanom Ghebreyesus of the World Health Organization called for an advisory panel to examine the ethical, social, and safety issues of the technology, saying that gene editing “cannot be just done without clear guidelines” and experts should “start from a clean sheet and check everything.” Also that day, Ed Yong in The Atlantic offered a meticulously researched roundup dissecting the many ethical boundaries that Dr. He and his still somewhat mysterious experiment crossed.
Everyone seemed to be in shock and awe, astonished, stunned, at the announcement of the gene-edited twins. But the clues had been accruing, making headlines, fleetingly, with each step. Even Dr. He reviewed them in his video: “While CRISPR/Cas9 has been studied in human cells and in early clinical trials, gene surgery in embryos intended for pregnancy has not previously been reported.”
This time, the headlines haven’t faded and seem to be ramping up. And that’s because of three words: “intended for pregnancy.”
 Sliding down the slippery slope
Sliding down the slippery slope
The precedents can be seen as building towards pregnancy, each experiment with a different target.
In May 2015, Junjiu Huang and colleagues, from Sun Yat-sen University in Guangzhou, used CRISPR/Cas9 to manipulate a gene that lies behind beta thalassaemia, an inherited anemia. Their intent wasn’t to create mutation-free babies, but to study the editing process and how it might go awry. The embryos that the researchers manipulated each had three nuclei – developmentally doomed to divide only a few times. Pregnancy was never intended.
Because several genes encode parts of the hemoglobin molecule, the controls are complex. The gene-editing experiments confirmed that challenge. The researchers concluded, “our work highlights the pressing need to further improve the fidelity and specificity of the CRISPR/Cas9 platform, a prerequisite for any clinical applications of CRISPR/Cas9-mediated editing.”
In August 2017 Shoukhrat Mitalipov, from the Center for Embryonic Cell and Gene Therapy at the Oregon Health & Science University, announced correcting a dominant mutation in a gene (MYBPC3) that causes a common form of heart failure, hypertrophic cardiomyopathy. The CRISPR components were introduced at the time of the application of sperm to the egg, so technically the action didn’t alter an embryo – it hadn’t yet formed, for it takes about twelve hours for the genetic packets of sperm and egg to meet and merge, establishing the new genome. Still, it’s altering the germline.
The early intervention was attempted to prevent mosaics from forming, which is when the engineered change gets into only some of an embryo’s cells. And it worked, for most of the embryos. The report was published August 2 in Nature, but MIT Technology Review broke the story July 26. (MIT Tech Review also broke this new chapter on November 25, which Antonio Regalado deduced from publicly available documents detailing the experiments ahead of the now-infamous YouTube birth announcement.)
In September 2017 came basic research from London, also reported in Nature, to investigate a gene, Oct4, which controls early embryonic development. “This is the first time that CRISPR-Cas9 genome editing has been used to study the function of a gene in human embryos, which can lead to improvements in stem cell biology, IVF treatment, and knowledge of how human embryos develop in the first window of seven days, perhaps revealing causes of when pregnancy fails,” said Kathy Niakan, a developmental biologist at the Francis Crick Institute in London and team leader (see “CRISPR opens window into early stages of human embryo development” at Genetic Literacy Project).
 Sowing the seeds of fear
Sowing the seeds of fear
Objections to Dr. He’s work centered on violating the sacrosanct ban on modifying a fertilized ovum, which would affect every cell in the developing body and be passed to the next generation. That’s not the same as the gene therapies that augment or correct somatic cells, like in the retina or blood cells, or even like a manipulation on an embryo that is more than a single cell. It’s the germline that rang the alarm bells.
Sketchy informed consent and the lack of published results in a peer-reviewed journal were also brought up.
Another objection was targeting the CCR5 gene, which is a receptor for certain pathogens. Eliminating or disabling it can block entry of HIV, but may let in other pathogens, such as West Nile virus. I think CCR5 was a logical choice for a proof-of-principle study.
But the bottom line behind the criticisms goes back to the “intended for pregnancy.” With the births, and those of a reportedly six other couples pending, the research is sliding down a slippery slope.
Those of us who recall the debut of modern biotechnology in the mid 1970s may have a more forgiving perspective. I tried to get that across, amid the uproar a few days after the announcement, in an interview for my local NPR station WAMC. (I got the call because I teach “Genethics” online for the Alden March Bioethics Institute at Albany Medical College.)
The gene editing reveal isn’t the first time widespread outrage has met an early use of a biotechnology. The reaction evokes the “triple-headed purple monster” mindset of 1976, when recombinant DNA technology was under heated debate. In February 1975, 150 molecular biologist superstars convened at Asilomar, on California’s Monterey peninsula, to explore the implications of combining genes of two species. The field started with insertion of genes from cancer-causing viruses into bacteria.
The Asilomar conference led to guidelines for “physical containment” via specialized hoods and airflow systems and “biological containment” to weaken organisms so that they couldn’t survive outside the lab. Today people with diabetes get their insulin from the drugstore, likely unaware that the drug is made in recombinant bacteria endowed with human genes. At one time, that idea was terrifying.
In 1985 came another giant genetics project that led to vigorous debate: sequencing “the” human genome. Millions of sequenced genomes later, some of us carry our genome sequences on our smartphones and are paid for sharing our information. But back in the late 1980s, the initial cost estimate was $1 billion.
The researchers who packed a room at the Cold Spring Harbor Laboratory on New York’s Long Island to debate the feasibility of the government’s version of the human genome project objected 5:1, ticking off their fears: diverting funding to fight HIV/AIDS, promoting data dumps rather than clever experiments. They compared the sequencing effort to climbing Mount Everest just because it’s there. In 1988 Congress authorized the National Institutes of Health and the Department of Energy to start sequencing. I’m glad Mount Everest won.
The current brouhaha against the gene-edited twins also echoes the recent history of alternative reproductive technologies.

In 1978, Louise Joy Brown, the first baby born of in vitro fertilization (IVF), was discussed as if she were a space alien until her ordinariness became apparent (see “My Life As the First Test-Tube Baby”). That’s similar to predictions that the gene-edited, HIV-free Lulu and Nana will be teased at school one day for the bit of genetic material and protein added to their one-celled-selves.
By now more than 8 million people share Louise Joy Brown’s origins in a dish. A decade after her birth came the first “savior sibling” when the Nash family used preimplantation genetic diagnosis (PGD) to conceive and select an embryo who would, one day, as Adam, provide stem cells to save his sister Molly from Fanconi anemia. The parents were vilified on talk shows. PGD is now commonly done with IVF to select the healthiest embryos.
Coda
Given the sagas of recombinant DNA technology, human genome sequencing, IVF and PGD, why does a new biotechnology – gene editing to prevent a health problem in people – elicit such strong reactions? Maybe because it combines the strategies of the past biotechnologies: Recombinant DNA adds genetic material to cells; IVF and PGD select cells receiving it. And of course Dr. He behaved in a dangerously renegade manner, eschewing ethics committees and even, according to the article in The Atlantic, devising a PR campaign.
I think that Dr. He’s experiments are perhaps well-intended, and editing out the HIV gateway an inspired target, with its precedent of safety as a natural variant.
Noted Harvard geneticist George Church was one of the few to at least consider, if not defend, Dr. He, pointing out that the Chinese children likely won’t die and the choice of CCR5 was to design a meaningful experiment, not replace antiretrovirals.
But Dr. He ignored international concerns, feeding a sometimes-sensationalized media view of the fledgling technology. (See “Viewpoint: Rampage movie offers twisted take on CRISPR gene editing” at Genetic Literacy Project.)
I hope that the Second Annual Summit on Human Genome Editing held last week in Hong Kong, where Dr. He described his work, as well as the comments from the WHO director, will serve as, or inspire, an Asilomar-like conference for gene and genome editing – a global one. Let’s learn from the past instead of panicking in the present.
Ricki Lewis is the GLP’s senior contributing writer focusing on gene therapy and gene editing. She has a PhD in genetics and is a genetic counselor, science writer and author of The Forever Fix: Gene Therapy and the Boy Who Saved It, the only popular book about gene therapy. BIO. Follow her at her website or Twitter @rickilewis































